Issues of thrombosis, bleeding, and transfusion are extremely common, and often complex, in critically ill patients.
Haematology in Critical Care: A Practical Handbookprovidesa dependable source of expert guidance on how to handle common haematological problems seen in the critical care setting, as well as the acute care of patients with a primary haematological disorder.
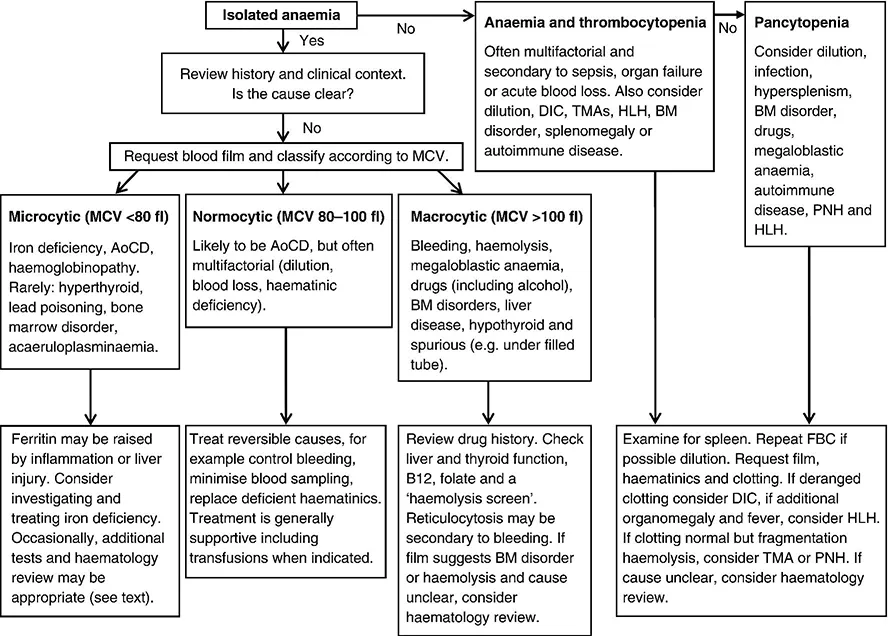
Full-time clinical haematologists, regularly attending on intensive care, the Editors begin with an approach to abnormal laboratory tests, following with a disease-orientated approach to topics such as coagulation and haematological malignancy. Other key topics include paediatric and neonatal care, transfusion, point of care testing and the emergency presentation of haematological disease.
This title brings together two of the most highly scientific specialties in clinical practice, delivering a practical approach to these problems, and guiding the clinician through the diagnosis and management of common scenarios encountered in the ICU.