![]()
1 Introduction
Climate change affects all geographic regions around the world. Its implication on health and well-being of human beings is an essential topic for public health and environmental health practice in the 21st century. Extreme temperatures, changes in precipitation patterns, and the rise of sea level, are some main environmental consequences of climate change that affect global health and the public health systems. Rapid urbanisation (two out of three people are expected to live in cities by 2030), population movement, ageing, and globalisation further complicate and exacerbate the public health impact of climate change on the one hand (e.g. urban heat island effect), while providing opportunities for mitigating this impact on the other (e.g. the smart city initiative). In addition, with surging of both frequency and severity of climate-related disasters, the understanding and preparation for related events will matter to the survival of individuals and communities in urban context.
This book presents a public health conceptual framework and the latest research findings of the climate change impact on human health in Hong Kong, a subtropical metropolis in Asia. It also aims to introduce essential concepts and methodologies in the field to non-specialists, as well as discuss local and global policy implications of climate change-related health impact. It will help readers understand, study, and discuss climate change impact on urban health in the context of public health; explore what could be done to minimise health impact of climate change from public heath perspectives; and appreciate recent research findings and local and global policies in relation to climate change and health.
The book starts with describing the basic concepts and principles of climate change, disaster, and public health. It goes on to discuss the association between climate change and natural disasters, trends of the occurrence of the climate change-related natural disasters, as well as the public health and vulnerability of the populations exposed to the risks, with a specific focus on urban subtropical Asian context. Issues regarding the challenges of health impact assessment and future extreme weather event trend prediction are also discussed. Research methodologies that are commonly used to study climate change and health impact will be examined. A substantial part of the book is devoted to discussing the latest research evidence in climate change health impact in terms of mortality, hospital admissions, help-seeking behaviours, adaptation, and mitigation in Asian urban settings. This book explicitly explains and applies public health concepts to examine the human impact of climate change, i.e. conceptualising climate change impact and its alleviation, mitigation, and adaptation in a public health framework.
Chapters 2 to 4 of the book provide an overview of the concepts of public health, climate, and its impact on health and well-being. Chapter 2 discusses the common theoretical principles that are useful for understanding the relationship among health, public health, and climate change. Chapter 3 examines the general health-related impact of climate change on human population. Chapter 4 describes how climate change might affect natural disasters. The following three chapters describe the study context and research methodology for the evaluation of health impact of climate change in urban context. Chapters 5 and 6 provide a general description of the research methodologies for impact-health outcomes modelling and climate in urban context. Chapter 7 describes Hong Kong as the main study context of research outcomes reported in this book. The subsequent three chapters present a range of studies related to analysing how health of population in Hong Kong, as a subtropical highly urbanised city, is being affected by climate change. Specifically, impacts of temperature on various health outcomes are examined. Chapter 8 describes the findings of how mortality is being affected by temperature, its extreme and urban heat island effect in Hong Kong. Chapters 9 and 10 further present findings of how temperature might affect various communicable disease-related hospitalisation outcomes and non-communicable disease-related hospitalisation outcomes in the city. Chapters 11 to 13 discuss how strategies and programmes in adaptation, mitigation, and policymaking might facilitate future planning and programme implementation to mitigate the adverse health outcomes for urban communities. Chapter 11 delineates help-seeking, health, and information-obtaining behaviours of at-risk communities in Hong Kong. Chapter 12 shares studies that inspect adaptation strategies that might be adopted from top-down (e.g. temperature warning from the authority) as well as bottom-up (e.g. self-help behaviours) approaches. Chapter 13 examines mitigation strategies with specific discussion of findings of health-environmental co-benefit (HEC) patterns in the local study context. Crucial global climate and health agreements such as the Sendai Framework for Disaster Risk Reduction 2015–2030, Paris Agreement under the United Nations Framework Convention on Climate Change, and New Urban Agenda (Habitat III) are explored. Chapter 14 is the epilogue of this book, which summarises and concludes the current knowledge of climate change and health in Hong Kong.
![]()
2 Principles of health, public health, and climate change
This chapter provides an overview of the common theoretical concepts in health, public health, and climate change. It highlights how the health implication of climate change might be conceptualised and potentially examined systematically.
Health and public health principles
Health and public health
World Health Organization (WHO) defined health as: “a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity” (WHO, 1946, p. 1). The definition includes both negative (e.g. illness and disease) and the positive dimensions of human well-being. It implies that there are always actions that may minimise diseases and maximise attainment of potential health (WHO, 1946). Whilst clinical medicine aims to protect health from diseases of individuals, public health focuses on approaches to protect and improve the health of communities and populations. Public health is defined as “[t]he science and art of preventing disease, prolonging life and promoting health through the organised effort of society” (Acheson, 1988, p. 1). Fundamentally, public health concerns about preventing and tackling health risks and challenges resulted from biophysical characteristics, human behaviour, and living environment.
The three domains of public health
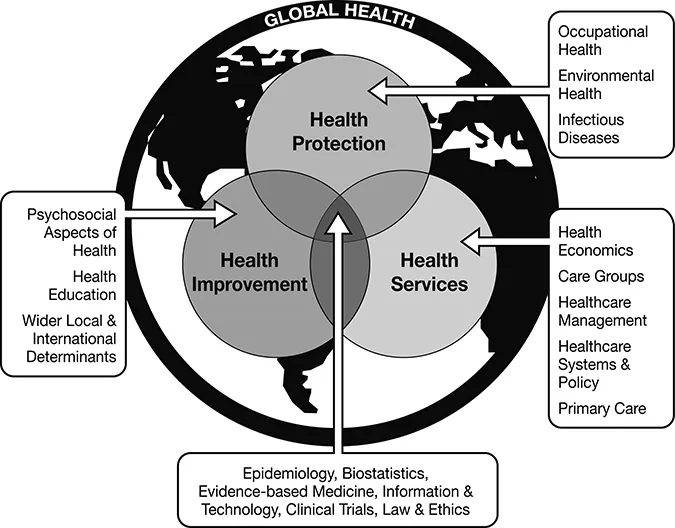
Academic subjects related to public health might be conceptualised in three key domains and their methodological approaches. Public health as a science-based academic/subject discipline is grounded with methodological branches such as epidemiology, biostatistics, law, and ethics, and research approaches such as clinical trials. Health protection describes the prevention and control of health risks and hazards. Examples of core topics in health protection include infectious diseases, the regulation and monitoring of environmental hazards, such as quality of air, water, and food, and response to chemical emergencies. Health improvement involves approaches and strategies that might improve health and well-being, as well as how health inequality may be reduced. Activities and interventions in health improvement often work best when multi-sectoral collaborative efforts with health are involved (e.g. education, housing, and social services). Health services identify the best ways to organise, deliver, and mobilise resources to address needs in policy and service arrangement (e.g. service planning, improving evidence-based practices, clinical effectiveness, governance, and resource allocation) (Frumkin, Hess, Luber, Malilay, & McGeehin, 2008; Griffiths, Jewell, & Donnelly, 2005). Figure 2.1 shows a conceptual diagram of how public health might be conceptualised.
Health determinants
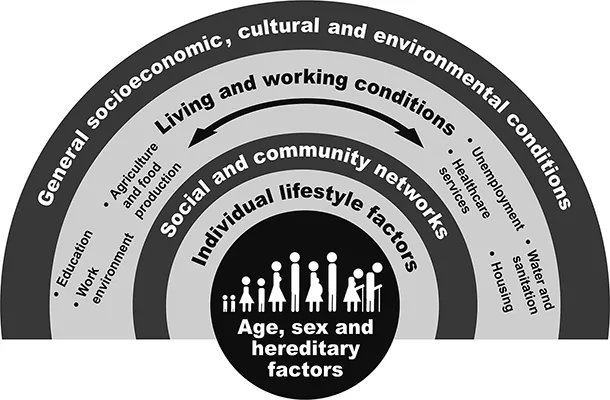
Health outcomes and well-being of individuals and communities are affected by multiple health determinants. Figure 2.2 illustrates the determinants of health. It hypothesises that individuals have only partial control over many of these determinants and whether people are healthy or not is determined by both modifiable and non-modifiable risk factors across one’s lifetime (WHO, n.d.). Non-modifiable health risk factors include age, sex (with physiological difference), and genetics (the likelihood of developing certain illnesses), while modifiable health risk factors involve personal belief, behaviour, and coping skills; dietary habit, exercise, smoking, and stress coping methods; income level and social status; education level; social support networks (e.g. availability of community support); context and location of residence; access to health service; and macro-determinants (e.g. cultural, religion, and political systems).
Figure 2.1 The three domains of public health.
Source: Chan (2017).
Figure 2.2 Determinants of health.
Source: Adapted from Dahlgren and Whitehead (1991).
Measuring health effects
Measuring health effects of a condition/context on a person or in a community requires the quantification of relationship between health outcome severity and the proportion of the population experiencing the effect/impact. Figure 2.3 shows how health outcomes might be affected by the same condition. Health outcomes may be measured in a diverse way. They can be assessed by physiological outcome measures (e.g. mortality rate and clinical symptoms), psychological aspects (e.g. depression patterns), or service utilisation outcomes as a result of impact severity (e.g. hospital admission rates...