The concept that the gut and brain are intricately linked is widely accepted not just within the lay community but increasingly within scientific and therapeutic circles as well. Terms such as "heartache" and "gut wrenching" are more than mere metaphor, they represent key fundamental aspects of human experience which all individuals will invariably endure from time to time. The relationship between the gut and brain is complex but fundamental to health and wellbeing. Increasing and compelling evidence supports the existence of a relationship between the health and status of the gut and the manifestation of significant psychopathology. Uniquely within the field of mental health and psychiatry, the role of gut flora and probiotics in both the understanding and treatment of mental illness represents an emerging science whether the potential for therapeutic intervention, through the use of probiotics, offers an opportunity to determine efficacy within a coherent evidence-based model of both action and pathology or, moreover, offers interventions that are comparatively benign compared to the side-effect profile associated with most drugs used to treat mental illness. Probiotics in Mental Health examines the role of probiotics in a range of clinical presentations associated with significant psychopathology and facilitates a reconsideration of how mental illness may be conceptualised within a coherent gut-brain model of health and wellbeing. Under the rubric of enhancing wellbeing rather than dwelling on illness and disease, this exciting new volume not only comprises the latest evidence in the field but also advocates an approach characterised by the understanding of mental disorder within an evidence-based model and the pursuit of mental health and wellbeing through the most benign of interventions.
- 162 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
Probiotics in Mental Health
About this book
Trusted by 375,005 students
Access to over 1.5 million titles for a fair monthly price.
Study more efficiently using our study tools.
Information
Contents
Dedication
Acknowledgment
Foreword
Preface
Chapter 1 Introduction: Probiotics and Psychopathology
Derek Larkin and Colin R Martin
Chapter 2 Probiotics and Chronic Fatigue Syndrome
Derek Larkin and Colin R Martin
Chapter 3 The Gut Microbiota, Health and Exercise
Marie Clare Grant and Julien S Baker
Chapter 4 Impact of Probiotics on Communication between the Brain-Gut: Implications for the Treatment of the Psychological Effects of Digestive Disease States
Melanie G Gareau, Colin Reardon, Kim E Barrett and Philip M Sherman
Chapter 5 Probiotics and their Effect on Maternal and Neonatal Health
Caroline J Hollins Martin and Colin R Martin
Chapter 6 Mechanisms of Action of Probiotics in Psychopathology
Moira S Lewitt
Chapter 7 Probiotics and Eating Disorders
Ursula Philpot
Chapter 8 Probiotics and Obsessive- Compulsive Disorder
Derek Larkin and Colin R Martin
Chapter 9 Probiotics and Depression
Derek Larkin and Colin R Martin
Chapter 10 Probiotics and Alcohol Dependency
Derek Larkin and Colin R Martin
Chapter 11 Probiotics and their Potential Effects on Schizophrenia Symptoms
Mick P Fleming and Colin R Martin
Chapter 12 Probiotics and Alzheimer’s Disease
Derek Larkin and Colin R Martin
Chapter 13 Probiotics and Autistic Spectrum Disorder
Derek Larkin and Colin R Martin
Chapter 14 The Probiotics Evidence-base Improving Quality through Innovation in Research Methodologies
Colin R Martin and Derek Larkin
Index
Editors Biography
Chapter 1
Introduction:
Probiotics and Psychopathology
Introduction
As you will read throughout the proceeding chapters Probiotics and Psychopathology are fascinating topics in their own right, but when combined they illustrate a complete and intriguing link between our gastrointestinal bacteria and the nervous system.
The concept that the gut and brain are intricately linked, and their interactions are to a large extent intuitive, are millennia old and are deeply rooted in our language (Mayer, 2011). Terms such as “heartache” and “gut wrenching” are more than mere metaphor, we feel the ache of love and loss in our chest and abdomen. We experience an orchestral repertoire of emotions in our hearts and stomachs in the form of muscle tightness, or increased heart rate, or abnormal contractions of the stomach— the emotional areas of our brain are inextricably connected to pain regions. The interlink or crosstalk between the gut and brain has revealed a complex bidirectional communication system that appears to help not only maintain gastrointestinal homoeostasis, but is also likely to affect our mental and emotional wellbeing (Emery and Coan, 2010).
The pathway linking the nervous system and the digestive system was first discovered in the nineteenth century and was subsequently labelled the enteric nervous system (Furness, 2008; Furness and Costa, 1987). The enteric nervous system is considered the third branch of the autonomic nervous system, and has been termed the ‘second brain’ (Gershon, 1998; Mayer, 2011). It shares a similar size, complexity, and similarity in neurotransmitter, and signalling molecules with the brain (Gershon, 1998; Mayer, 2011).
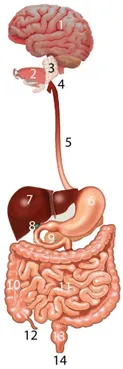
Figure 1 1. Human Brain, 2. Tongue, 3. Saliva Glands, 4. Pharynx, 5. Oesophagus, 6. Stomach, 7. Liver, 8. Gallbladder, 9. Pancreas, 10. Large Intestines, 11. Small Intestines, 12. Appendix, 13. Rectum, 14. Anus Figure adapted from https://www.britannica.com/science/human-digestive-system. (© 2003 encyclopedia Britannica, Inc.)
The interaction between the brain and the digestive system and their relationship with health and disease has been recognised for many centuries, and studied by ancient cultures, and in modern times by psychologists and physiologists (Mayer and Brunnhuber, 2012). There has been a long-term appreciation that there is an association between several chronic gastrointestinal tract disorders and psychiatric symptoms. While different theories have been proposed, the direction of causality and the precise nature of the underlying pathophysiology remains incomplete (Mayer and Brunnhuber, 2012). Nevertheless, recent scientific advances in the emerging fields of ‘enteric neuroscience’ and ‘emotional neuroscience’ have been instrumental in understanding the bidirectional brain-gut interaction (Mayer, 2011; Mayer and Brunnhuber, 2012). According to Mayer and Brunnhuber (2012) many clinicians continue to adhere to Cartesian dualism when treating patients with chronic gastrointestinal disorders. This idea implies that many gastroenterologists refrain from acknowledging the significant role played by the central nervous system in many disorders, which may include inflammatory bowel disease, or chronic oesophageal disorder. They dismiss psychological and psychiatric factors in the manifestation and maintenance of the disease process as neurotic hysterical behaviours which are only peripheral to the condition. In contrast psychologists and psychiatrics tend to embrace the concept of somatization; the manifestation of psychological distress by the presentation of bodily symptoms (Rhee et al., 2009). There is however still a rudimentary understanding of the involvement of the enteric microbiota including the commensal bacterial flora present within the gastrointestinal tract, which is part of the normal function of the gut. Consequently, the role of the enteric microbiota in the bidirectional gut-brain interaction in relation to general health and disease has received little empirical enquiry (Rhee et al., 2009).
The human digestive system is thought to be home to 400-1000 different species of bacteria, which make up an intricate network of cohabiting organisms (Mazmanian et al., 2008). The enteric microbiota can influence gut homeostasis by the regulation of bowel motility, modulation of intestinal pain, immune response, and nutrient processing (Ait-Belgnaoui et al., 2006; Husebye et al., 2001; Rhee et al., 2005; Rhee et al., 2009). There is a growing school of thought and mounting empirical research that is increasingly examining the symbiotic relationship between the enteric microbiota and their human host. This school of thought is driving afresh, an understanding of the importance of the two systems in maintaining homeostasis health (Turnbaugh et al., 2007).
Tremendous progress has been made in characterizing the bidirectional interactions between the central nervous system, the enteric nervous system, and the gastrointestinal tract. There is growing evidence of the fact that gut microbiota has a powerful influence on gut-brain interactions. There is also growing evidence of gut microbiota influence and development of emotional behaviour as well as stress and pain modulation, and brain neurotransmitter systems (Mayer et al., 2015). Pre- and probiotics have been used to modulate gut microbiota to measure multiple biological systems that may ultimately influence behaviour via the autonomic nervous system, but there is limited information as to how these findings may translate to human health or the disease state, involving the brain or the gut-brain axis. But evidence is mounting which suggests the symbiotic bidirectional brain-gut relationship has other important features that relate to not only our physical well-being but also our psychopathology, outlined in each of the preceding chapters.
Probiotics
The word ‘probiotics’ was derived many thousands of years after it was known that certain food supplements had beneficial effects. The etymology of ‘probiotic’ is derived from the meaning ‘for life’ in Greek, but has had several meanings over the years. Probiotic is in essence described as a substance that is secreted by one microorganism which stimulates the growth of another (Fuller, 2012). However, a more complete definition that was commonly accepted was first used by Parker (1974), organisms and substances which contribute to intestinal microbiota balance. Nevertheless, this definition was thought to have included all microbial substances including ‘antibiotics’ as such Fuller (19...
Table of contents
- Cover
- Halftitle Page
- Title Page
- Copyright
- Dedication
- Acknowledgment
- Foreword
- Preface
- Table of Contents
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.5M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1.5 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Probiotics in Mental Health by Colin R. Martin, Derek Larkin, Colin R. Martin,Derek Larkin in PDF and/or ePUB format, as well as other popular books in Psychology & Medical Microbiology & Parasitology. We have over 1.5 million books available in our catalogue for you to explore.