Chapter 1
Managerial epidemiology: Creating care of health ecosystems
Edward M. Rafalski
Contents
Introduction
What is epidemiology?
What is managerial epidemiology?
What is an ecosystem of care?
Social media and its application
Conclusion
References
Introduction
Managerial epidemiology combines the science of epidemiology with management principles applied to the improvement of systems of health, whether real or virtual.1 In this chapter, we explore the future of healthcare analytics from the perspective of studying disease using more recently available data sources to prepare healthcare systems, their analysts, and leaders to create more value for society and the individual consumer.
What is epidemiology?
Epidemiology is the study of how disease is distributed in populations and the factors that influence or determine this distribution.2 This definition assumes that disease is not random and that characteristics protect or predispose us to disease. It is also the study of the distribution and determinants of health-related states or events in specified populations and the application of this study to the control of health problems.3 It may also be the study of the distribution and determinants of health and disease in populations, including injuries, accidents, and violence, and the application of this study to promotion of health, prevention of disease, treatment of disease, planning for health and disease, and health policy.4 Distribution of disease refers to the who, when, and where of an outbreak. Determinants are characteristics that influence whether or not disease occurs. States and events refer to diseases, episodes, and disasters. Disease that affects the population affects a group, not just a single individual.
Regardless of which definition of epidemiology one prefers, the goal is for organizations to be better prepared to deal with future health events and to influence as many variables among target populations as possible to prevent or defer the onset of disease. It is a purpose of public health science and varies, most notably, from medical science given its focus on treating a population versus an individual.
What is managerial epidemiology?
Having a general understanding of epidemiology, the addition of the word “managerial” suggests the application of the principles and tools of epidemiology to the decision-making process in healthcare management. Just as in managerial accounting where the manager is using financial indicators to inform decision-making, the healthcare manager is gleaning information from epidemiological data to inform decision-making.
Integrating epidemiology and its methods into management approaches can be achieved through a number of organizational positions and roles. For example, in strategic planning, the planning analyst is typically looking into the future (usually in the 3- to 5-year horizon) and making recommendations to the organization regarding a suggested course of action based on the best information available on demographics, competitive and regulatory forces, and disease incidence in a target market or population. In staffing and organizing, the human resources analyst is considering how the incidence of disease may influence the need for additional resources. In finance, the analyst is considering the scale of resources required to meet the need or demand for services based on changes in disease incidence in order to calculate a financial return on the investment made. In marketing, the analyst is considering how to motivate the consumer from a precontemplative to a contemplative state and ultimately to act on his or her own health, in other words, to make a healthcare purchase in advance of developing the disease or in the course of managing a chronic condition. In each case, epidemiological data serves as the reference point for informed organizational decision-making.
What is an ecosystem of care?
When thinking about the prevention of disease, segregating the effort into primary, secondary, and tertiary prevention is useful. Primary prevention is focused on avoiding disease altogether, generally by preventing disease development.5 Weight management/obesity prevention as a precursor to onset of chronic disease, such as hypertension and type II diabetes, is an example. Secondary and tertiary prevention are primarily focused on addressing an illness once it has manifested.
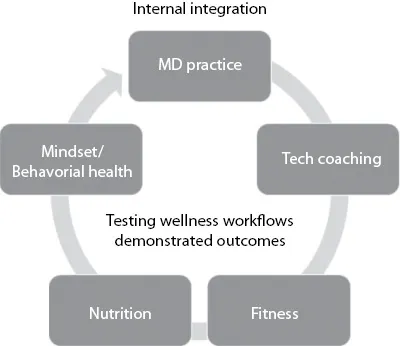
In the primary prevention effort to prevent the onset of obesity, appropriate amounts of diet and exercise can contribute to a successful prevention strategy. When considering how a traditional healthcare system approaches this prevention strategy, assets that are owned or controlled are typically positioned to intervene with the patient in an effort to change behavior. Processes are tested using reliable methodologies, such as Lean/Six Sigma,6 to standardize workflows, eliminate waste, and achieve consistent outcomes. An example of this approach may include core elements such as primary care, coaching, fitness, nutrition, and mindset/behavioral health (Figure 1.1). Data is captured at each nodal point and integrated into a data warehouse/repository structure enabling the analyst to query the data set to determine outcomes in target populations.7,8 This is a common model in many health systems across the United States with various flavors and permutations. Some call this population health or accountable care.
Figure 1.1 Ecosystem of care.
However, the model may have a flaw—healthcare consumers spend more time outside of the healthcare system, on average, than inside of it, thereby limiting the potential for high engagement and meaningful behavioral change. To place the problem in context, consider the following. The average healthcare consumer has an encounter with a health system/provider two to three times per year (within Medicare, the national insurance program for the elderly and disabled, consumers may have four to five encounters). The average grocery shopper may be in the store one to two times per week. Nearly one in five Amazon shoppers are on the site every day making purchases or contemplating purchases.9
Consider the primary care annual physical encounter, which typically is an event lasting 15 minutes or less, as an opportunity to generate patient engagement. In that small window of time, a patient at risk for hypertension is encouraged to change behavior, prior to being prescribed a drug(s), depending on where the patient lies on the “disease spectrum.” Family history/genetic markers of the disease may lead the physician to be more aggressive in recommending a course of treatment. The patients’ spectrum position may lead to the application of additional resources to help the patient reach a goal set by the physician. In accountable care organizations or vertically integrated health systems with a health plan, resources the physician may call on include case/care management. Care management is a set of activities intended to improve patient care and reduce the need for medical services by helping patients and caregivers more effectively manage health conditions. Case management is the coordination of services on behalf of an individual. Unfortunately, case/care management resources are typically reserved for the more chronically ill, qualifying the effort as secondary prevention. What can be done to move the effort to primary prevention?
Case for primary prevention and care of health ecosystem
It has been well established that Americans consume a majority of medical resources in the last 2 years of life.10 Arguably, our national resources can be better spent earlier in life to prevent unnecessary expenditures at the end of life and thereby lead to a higher quality of life.11 Unlike he...