'The Quality and Outcomes Framework (QOF) is a system to financially reward general practices for providing quality care to their patients. It is a fundamental part of the GMS contract, introduced in April 2004. QOF is estimated to have saved up to 10, 000 lives a year since its introduction - ' - From the Preface Filled with practical guidance and tips, this book explains everything you need to do in order to score 'maximum' on all the clinical indicators in the QOF. Using tables and lists, it details areas such as setting up a disease register, ensuring that you have an accepted definition of the condition, arranging a practice meeting to discuss registers and motivating team members to use and think about templates as well as cross-checking hospital letters and discharges summaries, conducting a repeat prescription search, actively screening at-risk patients and ensuring an efficient call and recall system. These are the basic rules which apply to any and every clinical indicator. Offering guidance on and insight into the origins of different targets, possible shortfalls, and ways to implement change and improve scores, this easy-to-read book is vital for all general practitioners, GP Commissioners, QOF assessors, and PCT QOF teams. Practice nurses, who are often relied upon to maintain QOF standards, will find the information essential. GP Registrars, medical students, Pharmacists, Health Care Assistants and Practice Managers will also find much of interest.

eBook - ePub
Maximising Quality and Outcomes Framework Quality Points
The QOF Clinical Domain
- 220 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
About this book
Trusted by 375,005 students
Access to over 1.5 million titles for a fair monthly price.
Study more efficiently using our study tools.
Information
CHAPTER 1
QOF clinical indicators: 2009/10
The Quality and Outcomes Framework (QOF) was introduced as part of the 2004 GP contract. It currently offers practices up to 1050 points if the delivery of care is of a high standard on a range of services. Payments per point vary with relative practice prevalence and the patient list size. In 2004/05, payment was £77.50 per point, yielding £80 000 per annum potential gross income. In 2005/06, this was increased to £124.60 per point, yielding a potential gross income of £130 000 per annum for average sized practices.
New indicators were added in 2006, 2008 and 2009/10, with further changes planned for 2011/12. The points are linked to the clinical and organisational structure and patients’ experience of the practice.
Each QOF point is currently worth £127.29. The practice agrees in advance with the primary care organisation the total number of QOF points it is aiming for in the coming year. Seventy per cent of the payment is made to the practice on a monthly basis, with the balance being paid once the practice has proved that the target points have been achieved.
The QOF of the general medical services (GMS) contract for 2009/10 came into effect on 1 April 2009. The clinical domain covers the areas shown in Table 1.1.
Table 1.1 Quality and Outcomes Framework: clinical domain categories, 2009/10
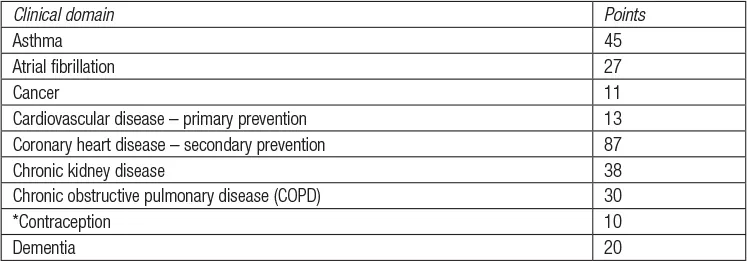
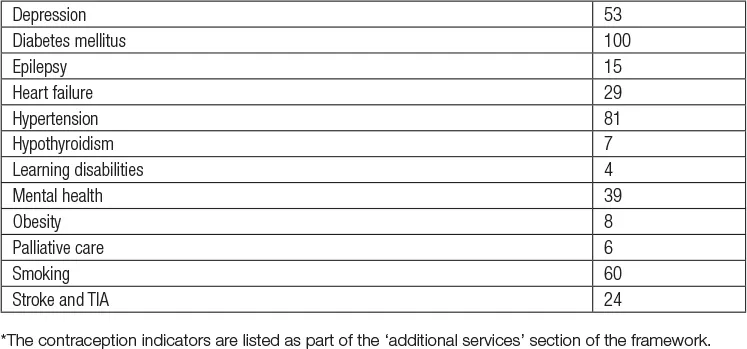
Points are attached to each indicator and the number of points achieved determines the sum earned.
All clinical indicators are organised by disease categories. The QOF expects the primary care physician to provide a high quality of care in the categories listed in Table 1.1.
These categories were selected on the basis of good evidence of the health benefits from improved primary care, and where the disease area is a priority because of the substantial burden, in terms of morbidity and healthcare expenditure in particular, and if there is an accepted national clinical guideline.
The indicators chosen are largely process based, and much of the effort in earning points boils down to good data collection. The framework endorses the advice of the guidelines on the specific disease to make an objective diagnosis.
The key aims of QOF clinical indicators are to:
- prevent the disease developing in the first place
- slow down the progression of the disease
- make an early diagnosis and provide ongoing management as per accepted national guidelines by the primary care team
- reduce the complications associated with the disease
- reduce hospital admissions and deaths by providing better primary care.
The incentive to improve diagnosis is contained in the process of prevalence. Once diagnosed the patients should receive timely and appropriate investigations, with effective treatment and follow-up by the primary care team to reduce the risk of progression and complications.
In 2009/10, 72 points were removed from the following indicators, as shown in Table 1.2.
Achievements in the clinical domain of the QOF fell from 97.8% in 2008/09 to 95.9% in 2009/10 with scores markedly lower in the newest indicators introduced in the last round of negotiations including diabetes and depression screening. Average practice achievement in the 8305 practices in England was 93.7% of all QOF points available, equivalent to a £2125 loss for the average practice. The DM23 indicator (percentage of patients with diabetes in whom the last HBAlc is 7% or less in the previous 15 months) scored the lowest of all clinical indicators, with practices scoring 83.5% of the points available. The National Institute for Health and Clinical Excellence (NICE) has recommended increasing this target to 7.5% from next year. Another indicator where practices scored less was DEP3. Practices scored only 64.4% of the points available for DEP3, which offers 20 points for the percentage of patients who are reassessed 5-12 weeks after the first assessment of depression and anxiety severity using a validated assessment tool.
Table 1.2 Quality and Outcomes Framework: indicator points removed, 2009/10
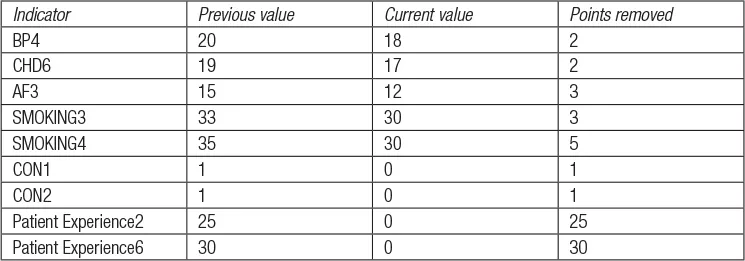
It is proposed that NICE should be involved in reviewing existing indicators and piloting new indicators. This has been welcomed by GPs because the achievement of the target of some of the indicators is currently impossible.
QOF changes and new indicators
The following new indicators will be reviewed prior to the start of 2011/12.
Anxiety and depression: one new indicator worth 20 points
DEP3
In those patients with a new diagnosis of depression and assessment of severity recorded between the preceding 1 April and 31 March, the percentage of patients who have had a further assessment of severity 5-12 weeks (inclusive) after the initial recording of the assessment of severity. Both assessments should be completed using an assessment tool validated for use in primary care.
Points 20 Thresholds 40-90%
Primary prevention of cardiovascular disease: two new indicators worth 13 points
PP1
In those patients with a new diagnosis of hypertension (excluding those with preexisting coronary heart disease (CHD), diabetes, stroke and/or transient ischaemic attack (TIA)) recorded between the preceding 1 April and 31 March, the percentage of patients who have had a face-to-face cardiovascular risk assessment at the outset of diagnosis using an agreed risk assessment tool. At the outset of diagnosis means as within three months of the initial diagnosis.
Points 8 Thresholds 40-70%
PP2
The percentage of people diagnosed with hypertension diagnosed after 1 April 2009 who are given lifestyle advice in the preceding 15 months for increasing physical activity, smoking cessation, safe alcohol consumption and healthy diet.
Points 5 Thresholds 40-70%
Diabetes: 7 new points plus 28 current points
DM23
Replaces DM20. The percentage of patients with diabetes in whom the last HBA1c is 7 or less (or equivalent test/reference range depending on local laboratory) in the previous 15 months. ^
Points 17 Thresholds 40-50%
DM24
New. The percentage of patients with diabetes in whom the last HBA1c is 8 or less (or equivalent test/reference range depending on local laboratory) in the previous 15 months.
Points 8 Thresholds 40-70%
DM25
This replaces DM 7. The percentage of patients with diabetes in whom the last HBA1c is 9 or less (or equivalent test/reference range depending on local laboratory) in the previous 15 months.
Points 10 Thresholds 40-90%
COPD: 2 new points, one revised indicator
COPD 13
Replaces COPD11. The percentage of patients with COPD who have had a review, undertaken by a healthcare professional, including an assessment of breathlessness using the MRC dyspnoea score, in the preceding 15 months. Two additional points.
Points 9 Thresholds 50-90%
Heart failure: 9 new points, one new indicator
HF4
The percentage of patients with a current diagnosis of heart failure due to LVD who are currently treated with an ACE inhibitor or angiotensin receptor blocker, who are additionally treated with a beta blocker licensed for heart failure, or recorded as intolerant to or having a contraindication to beta blockers.
Points 9 Thresholds 40-60%
CKD: 11 new points
CKD5
The percentage of patients on the CKD register with hypertension and proteinuria who are treated with an angiotensin converting enzyme inhibitor or angiotensin receptor blocker unless a contraindication or side-effects are recorded.
Points 9 Thresholds 40-80%
CKD6
A new indicator added: the percentage of patients on the CKD register whose notes have a record of an albumin: c...
Table of contents
- Cover Page
- Title Page
- Copyright Page
- Contents
- Foreword by Shauna Dixon
- Foreword by Tanya Claridge
- Preface
- About the author
- Acknowledgements
- 1 QOF clinical indicators: 2009/10
- 2 How to achieve maximum QOF points
- 3 QOF: Good or bad?
- 4 Points and pounds
- 5 Asthma
- 6 Atrial fibrillation
- 7 Cancer
- 8 Cardiovascular disease: primary prevention
- 9 Coronary heart disease: secondary prevention
- 10 Chronic kidney disease
- 11 Chronic obstructive pulmonary disease
- 12 Long-acting reversible contraception (LARC)
- 13 Dementia
- 14 Depression
- 15 Diabetes mellitus
- 16 Epilepsy
- 17 Ethnicity
- 18 Heart failure
- 19 Hypertension
- 20 Hypothyroidism
- 21 Learning disability
- 22 Mental health
- 23 Obesity
- 24 Palliative care
- 25 Smoking
- 26 Stroke and TIA
- 27 Alcohol: directed enhanced service
- 28 QOF: the assessment process
- Index
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.5M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1.5 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Maximising Quality and Outcomes Framework Quality Points by Anita Sharma in PDF and/or ePUB format, as well as other popular books in Medicine & Service Industry. We have over 1.5 million books available in our catalogue for you to explore.