![]()
Chapter 1
Introduction
Efficiency and Effectiveness Issues
Efficiency and effectiveness are two key words in organizational activities. An organization is said to be efficient if it is able to use all of its resources to produce something valuable without leaving undesirable things. Meanwhile, an organization is said to be effective if it is able to perform in line with what is expected of the organization. These criteria should also be applied to hospitals as organizations in the health system.
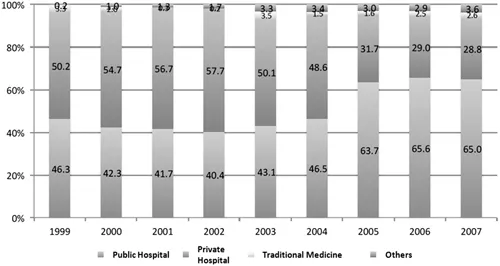
A number of efficiency and effectiveness issues can be found at the hospitals in Indonesia. Antibiotics are still inefficiently given to 44%–97% of hospital patients regardless of their need or the appropriateness.1 In addition, current hospital utilization has tended to decline since 1997.2 This is due to developments in information technology that encourage people to rely more on self-medication, with various types of drugs available from drug stores or pharmacies. Communities view going to the hospital as more complicated because they must register, wait in line, and pay the consultation fee. Meanwhile, self-medication is seen to be as effective as hospital services in terms of the achievement of the goal to obtain a patient’s health, at least for ailments. This is shown in Figure 1.1.
Figure 1.1 Community options for treatment facilities. (From Indonesia’s Doctors, Midwives and Nurses: Current Stock, Increasing Needs, Future Challenges and Options. Washington, DC: World Bank, 2009, p. 22.)
The increasing number of people who seek treatment at health care facilities provides a surge in demand that is too large for public hospitals. Meanwhile, in terms of human resources, decentralization leads to the duplication of tasks and functions, causing inefficiencies of duty implementation.2 On the other hand, the hospital accreditation system has at least three problems: (1) conflict between the government’s role as regulator and assessor, (2) greater focus on input indicators, and (3) lack of integral development.3
The Model of Lean Healthcare
Lean is an efficiency improvement model for organizations that is widely used by hospitals today. Lean principles have been gaining great attention since 1990,4 when Womack, Jones, and Roos published the book The Machine That Changed the World, which later became a best Lean seller.5 The term Lean itself was popularized in 1996.6 Four years later, Lean started to be implemented in service areas around the world. Lean was introduced into healthcare service in the early 2000s.7 Throughout the decade, Lean was researched and tested together with other models. In the end, Lean tended to show more ability when applied in the healthcare industry.5 In line with these trends, Lean has also reached the strategic realm; it is no longer just in the operational realm.5 The appointment of Lean in the strategic realm was motivated by research results that found a relationship between Lean implementation and strategic aspects. Strategic aspects include operational management, employee health and quality of life,4 competitive advantage,5 and organizational learning.8 Since then, Lean has attracted various industries throughout the world and is being applied in many operational aspects besides manufacturing.9
From here on, we discuss the model of Lean healthcare. Lean healthcare is defined as the “elimination of waste in every field of activity with the aim to reduce inventory, cycle of service time, and cost. So in the end high-quality patient care can be provided in a way that is as efficient, as effective, and as responsive as possible, while retaining economical eligibility of organizations.”10 The model of Lean hospitals, then, briefly interpreted, is hospitals that implement Lean.
The Benefits of Lean Hospitals
The new Lean principles were thoroughly applied in three pioneer hospitals in 2005: Virginia Mason in Seattle, Washington, Flinders in Adelaide, Australia, and ThedaCare in Appleton, Wisconsin.11 Lean projects successfully showed progress in the hospitals. After that, Lean implementation penetrated various hospitals around the world, and study results show that positive cases related to Lean implementation in hospitals are increasing.
Although Lean focuses on cost reduction and process flow, this focus is the same with sustainable development.12 Lean and sustainable development have a point of agreement. The meeting point is located at the operational focus in the form of waste reduction.12 Both sustainable development and Lean equally attempt to reduce waste as much as possible, which means increasing efficiency.
Some empirical evidence has shown the benefits of Lean for hospitals. Vliet et al. in 2010 conducted a study in the cataract clinic at the Rotterdam Eye Hospital in the Netherlands.13 They found that Lean lowered repeat outpatient procedures by 23% and increased patient access by 42%. Similarly, a study by McCullock et al. in 2010 found that the number of referred patients decreased 7%, from 27% to 20%. It is also found that the number of patients increased from 969 to 1114 at a university hospital in the United Kingdom.14
In terms of cost savings, a number of studies by Womack et al. at the Virginia Mason Medical Center, report savings of $1 million on hyperbaric examination.15 In addition, there has been a $1–$3 million savings on endoscopy and $6 million on surgery. A $7.5 million savings in insurance costs was found in studies at Park Nicollet Health Services, Minneapolis, Minnesota.16 A similar study in LeBonheur Children’s Medical Center, Memphis, found a $243,828 savings in supplies.17
Empirical evidence regarding the relationship of Lean thinking with service time savings was reported by Taninecz in 2004.18 Taninecz reports that the response time and emergency services time are accelerating at Hotel-Dieu Grace Hospital, Windsor, Ontario, Canada. Studies of Melanson et al. in 2009 at Brigham and Women’s Hospital, Boston, Massachusetts, found that after Lean implementation, the waiting time for laboratory examination decreased from 21 ± 3 minutes to 11 ± 5 minutes.19
The efficiency aspect in terms of the work area can also be improved using Lean practices. The studies of Womack et al. in 2005 report that Lean implementation at the Virginia Mason Medical Center reduced the work area 35%–50%.15
Actually, there are many other philosophies that can be applied aside from Lean—from the most conventional, standardized systems to the theories of advanced management. From the various formal approaches, there is not one that is superior to the others in all contexts. Each has its own strengths and weaknesses.20 Indeed, the batch-and-queue system has weaknesses,21 but it is likely to be easier to apply. Meanwhile, the Uddevalla method, despite encouraging team and individual learning, limits organizational learning and system improvement on the whole.22
A standardization system, while not sensitive to context, needs to be the basis of quality. In the meantime, a continuous quality improvement system demands a capable human resources infrastructure, but it can have a majo...