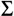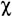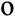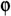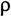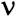Definition
The term
schizophrenia was coined by Eugen Bleuler in the early twentieth century, and is derived, somewhat unhelpfully, from the Greek
schizo-(
ı
=split/divide), and
phrenos (
o=mind). Perhaps owing to this etymology, the words ‘schizophrenia’, and especially ‘schizophrenic’, have acquired a completely unrelated colloquial usage, whereby they are used to refer to a paradox or contradiction. More troublingly, many people hold the erroneous belief that people with schizophrenia have a ‘split personality’ or are subject to sudden dangerous transformations from normality to madness, similar to the character of Dr Jekyll and his alter-ego Mr Hyde, in the Victorian novella by Robert Louis Stevenson (Stevenson, 1886).
The modern concept of schizophrenia is based on Emil Kraepelin’s descriptions of dementia praecox, which in turn drew on previous accounts by Haslam, Morel, Pinel and others (Adityanjee et al., 1999). Schizophrenia is a severe and chronic mental disorder, which usually manifests itself in early adulthood, and is characterised by a disparate range of symptoms, which despite their superficial unconnectedness, frequently co-occur in the same individual.
The most obvious symptoms to most observers are the so-called positive symptoms. Hallucinations (perceptions without an external source) occur in almost all cases. These include auditory hallucinations (primarily hearing voices), although hallucinations are sometimes also experienced in other sensory domains, such as touch or smell. A second feature that is almost universal is the presence of delusions (fixed, false beliefs, which are out of keeping with the person’s cultural background), and these are commonly paranoid or persecutory in content. Disorganised and erratic behaviour is frequent, as is thought disorder (severely disjointed or tangential connections between thoughts, and idiosyncratic vocabulary and grammar, manifesting as speech that is difficult to follow or even unintelligible). Over time, and often beginning before the onset of the positive symptoms described above, there is, in most cases, a marked deterioration in occupational and social functioning, often described as ‘negative symptoms’.
Is schizophrenia a valid concept?
There has been fierce debate for over a century as to whether schizophrenia exists at all, whether it constitutes a single disorder or a collection of disorders, to what extent it can be demarcated from other disorders, and whether it is separable from normal functioning categorically, or only by degree. At the heart of all these debates lies the fundamental question of what defines a disease, and the uncomfortable truth that the causes and neurobiological basis of schizophrenia remain obscure.
Although there is clear evidence from many fields of research, including genetics, pharmacology, neuroimaging and epidemiology, that patients with schizophrenia differ on average from the remainder of the population, there is not, and may never be, an unambiguous biological ‘test’ that can reliably differentiate between people with a diagnosis of schizophrenia and healthy individuals. Instead, the diagnosis of schizophrenia is based on signs and symptoms. Signs are the clinician’s observations of the appearance, behaviour or speech of the patient (such as ‘this patient appears to be responding to hallucinations’). Symptoms are experiences volunteered by the patient, (such as ‘I can hear a voice echoing my thoughts’). In fact, it is more accurate to say that symptoms are the diagnostician’s evaluation of the patient’s own account of his/her perceptions, experiences and beliefs. Thus, schizophrenia, like most psychiatric ‘diagnoses’, is more accurately described as a syndrome (a group of signs and symptoms that frequently co-occur) than a disease. It is also important to note that the assessment of signs and symptoms involves many subjective judgements on the part of the diagnostician, and often also on the part of the patient.
Scientific definition
The subjective nature of psychiatric diagnosis was highlighted by the antipsychiatry movement in the 1960s and 1970s, and became a source of embarrassment to psychiatrists. Furthermore, it became clear that research efforts in identifying causes and treatments for mental disorders were being hindered by lack of consistency in the way that these disorders were defined. The response to this problem was to develop formal diagnostic criteria for mental disorders, which would be as objective and reliable as possible.
There are currently two dominant standards in Western psychiatry for the classification of psychiatric disorders: the International Classification of Disease, currently in its tenth edition (ICD-10), administered by the World Health Organization (WHO, 1992), and the Diagnostic and Statistical Manual of Mental Disorders, currently in its fourth edition (DSM-IV), published by the American Psychiatric Association (APA, 1994).
ICD-10 defines schizophrenia as follows:
This is followed by more specific diagnostic criteria for the various subtypes of schizophrenia.
The existence of these subtypes reveals another aspect of schizophrenia that dogs research efforts: its clinical heterogeneity, or variability. Two individuals with no overlap in their symptoms might both be diagnosed with schizophrenia, whereas another patient may suffer from auditory hallucinations at one time, then apathy and reduced social functioning years later, yet retain the same diagnosis throughout. Attempts have been made to subdivide the syndrome into separate subgroups based on symptom clusters. The DSM and ICD classifications both include the subtypes of paranoid, disorganised, catatonic, undifferentiated and residual schizophrenia. Although these subtypes have a rich history, they do not seem to aggregate within families or predict prognosis (Kendler et al., 1994). More recently, attempts have been made to use statistical techniques such as factor analysis to generate subtypes, such as the ‘deficit syndrome’ (Kirkpatrick et al., 2001), but the level of agreement as to what constitutes these subsyndromes is even less than for the overall syndrome of schizophrenia itself.
It is an interesting and useful exercise to consider what would happen if a completely naïve observer—the proverbial visitor from another planet— were to attempt a fresh classification of mental illnesses. Would he arrive at anything resembling the ICD or DSM? His classification would not necessarily be any better than ours, but I believe it would almost certainly be different. It is very likely that the classification would include at least one category of illness that shared many of the features of schizophrenia, since a large proportion of individuals receiving mental health care hear voices, harbour delusions and display deterioration in social functioning. However, it is possible to imagine many potential classifications that subdivided schizophrenia into many different but related disorders, and others that used a broader concept of schizophrenia (perhaps similar to the concept of ‘psychosis’ described below). Dimensional rather than categorical descriptions have been suggested, where individuals are seen as lying on a continuum between a complete absence of psychotic symptoms to severe illness.
How much does it matter how we define schizophrenia? My view is that many of the classifications proposed are more or less equally valid in scientific terms, so in some senses the question of how to classify schizophrenia could be viewed as a somewhat tedious and parochial debate among mental health professionals and researchers. However, there are two important areas where I believe that the definition of schizophrenia does matter.
The first is the problem of stigma. The label of schizophrenia is almost always seen in negative terms by patients and members of the public. To some extent this is inevitable, since, like cancer or stroke, schizophrenia is a devastating illness that has few, if any, positive aspects.
Some advocate changing the name of schizophrenia to something more palatable, although I am not convinced that this would have any more than a temporary impact on stigma, and it would inevitably create confusion. However, I would argue that because of the stigmatising nature of the illness, clinicians have a moral duty to ensure that the diagnosis is used as cautiously and precisely as possible.
The second problem is scientific validity. Unless researchers and clinicians can agree on an accepted definition, it is impossible to be sure that the results of a particular experiment or clinical trial are applicable to a particular patient, which is clearly vital if research is to have any clinical relevance.
In future, improved understanding of the genetics and aetiology of mental illnesses may allow us to devise a more valid classification. Until then, I believe the most pragmatic solution is to adhere as closely as possible to the clinical syndrome described in the classification systems. This at least has the advantage of maximising reliability (the extent to which different researchers are studying the same entity). This is essential if research is to add to an existing body of knowledge and be generalisable to clinical populations. However, it is important always to bear in mind that the concept of schizophrenia that we are employing is merely our current attempt to conceptualise a complex and confusing set of signs and symptoms, and to balance sometimes competing clinical, scientific and social priorities. Our concept of schizophrenia will probably evolve or be replaced as our knowledge and understanding of the disorder increases.