eBook - ePub
Actinic Keratosis
- 154 pages
- English
- ePUB (mobile friendly)
- Available on iOS & Android
eBook - ePub
Actinic Keratosis
About this book
In some respects actinic keratosis is the most common and best-known pathology in dermatology. Being such an ordinary pathology, actinic keratosis gives nevertheless insight into an extraordinary number of important biological and clinical processes. Actinic keratoses are found in significant numbers on the sun-exposed skin of Caucasians, especially those living in sun-bathed countries such as Australia, as two of the editors and a considerable number of the authors of this book do. The authors who have contributed to this volume are researchers and clinicians discussing actinic keratosis across the whole spectrum – from epidemiology to immunology, from molecular biology to behavioral psychology – and of course pathologists and clinicians dealing with patients who experience the many manifestations of actinic keratoses. The fact that all these various aspects are considered renders this book valuable reading for scientists and clinicians alike.
Tools to learn more effectively

Saving Books

Keyword Search

Annotating Text

Listen to it instead
Information
Soyer HP, Prow TW, Jemec GBE (eds): Actinic Keratosis.
Curr Probl Dermatol. Basel, Karger, 2015, vol 46, pp 49-57 (DOI: 10.1159/000366535)
Curr Probl Dermatol. Basel, Karger, 2015, vol 46, pp 49-57 (DOI: 10.1159/000366535)
______________________
Keratinocyte Cancer and Its Precursors in Organ Transplant Patients
Daniella Jenni · Günther F.L. Hofbauer
Department of Dermatology, University Hospital Zürich, Zürich, Switzerland
______________________
Abstract
Organ transplant recipients (OTRs) have a 65-to 250-fold increased risk of the development of cutaneous squamous cell carcinoma in the wake of immunosuppression. The combination of ultraviolet light and properties of immunosuppressive drugs potentiate skin cancer formation. Due to decreased peritumoral inflammation, the thickness and invasion of epithelial skin lesions are often underestimated clinically. Rapid tumor progression and aggressive tumor behaviors occur frequently in the OTR population. Tenderness and pain in a skin lesion may indicate its potential invasion beyond the basal membrane and the need for surgical removal. All patients should receive extensive education on ultraviolet avoidance and protection. In particular, a preventive and aggressive treatment of actinic keratosis in areas of field cancerization is recommended to cut down on the high morbidity and avoid the mortality associated with actinic keratosis and invasive squamous cell carcinoma in OTRs.
© 2015 S. Karger AG, Basel
Background
Progress in drug-induced immunosuppression and improvements in surgical techniques over the last decades have increased the number of solid organ transplantations as well as long-term survival in the organ transplant recipient (OTR) population [1]. At the same time, the side effects of continued immunosuppressive medications impair the benefits of organ transplantation, particularly including a markedly increased risk of malignancies in general and cutaneous intraepithelial and invasive epithelial lesions. Cutaneous squamous cell carcinoma (SCC) is the most frequent malignancy found in solid OTRs [2-8]. The risk of developing SCC in this population is up to 65- to 250-fold higher than in the general population, and SCC occurs roughly fifteen years earlier in OTRs [5, 7-10]. The risk of epithelial skin cancer accelerates in a linear fashion starting at the time of transplantation [7, 10-12]. The incidence of basal cell carcinoma (BCC) is elevated in OTR as well, albeit at a lower level (10- to 16-fold increase). Interestingly, while BCC is the most frequent skin cancer found in the general population followed by SCC at a ratio of 4:1, this ratio is inverted in OTRs [3].
Several risk factors for the development of intraepithelial and invasive epithelial tumors in OTRs are similar to those found in immunocompetent patients, such as age, male gender, and susceptibility to sunburn, and the main factors include high cumulative sun exposure and fair skin type (skin types I-III) [13, 14]. Several studies have also described a higher risk of SCC in OTRs with a high burden of viral warts and hyperkeratotic lesions [13, 14]. A correlation of SCC with human papilloma virus (HPV) has been suggested but not confirmed. The detection of high levels of HPV DNA in the SCC of OTRs suggests that HPV may play a role in the formation of SCC, especially in these patients [15, 16]. However, recent data have clearly shown that keratinocyte infection by HPV is a transient phenomenon [17]. The best current hypothesis is that transient HPV infection impairs the repair of DNA damage caused by ultraviolet (UV) light, thus favoring the development of epithelial skin cancer down the road.
The incidence of non-melanoma skin cancer depends on the dose of immunosuppressive medication as well as the type of immunosuppressive regimen. Immunosuppressive drugs accelerate SCC development by two pathomechanisms as follows: first, the resulting chronic immunosuppression creates a state in which immune surveillance and the eradication of aberrant cellular lesions are impaired [18]. Second, the medication may be directly carcinogenic, inducing phenotypic and functional cell changes, including the invasiveness of non-transformed cells [19].
The risk of SCC development in OTRs increases exponentially with time after transplantation. The mean time of occurrence of the first SCC is estimated at approximately 5-8 years post-transplantation [5, 6, 8]. In OTRs, the risk of SCC increases with a longer duration of transplantation, a younger age at the time of transplantation and an increased dose of immunosuppressive medication. Due to a relatively higher dose of immunosuppressive medication, lung and heart transplant recipients have the highest incidence of SCC, followed by kidney and then liver transplant recipients [7, 20-22]. OTRs following a triple immunosuppressive regimen consisting of cyclosporin, azathioprine and prednisone have a higher risk of SCC than those on bitherapy [23]. Some data have also suggested a higher risk of SCC development in patients on azathioprine independent of other co-medications [13]. The mTOR inhibitors sirolimus and everolimus are members of a newer class of immunosuppressive agents [24]. Several studies have presented convincing evidence that patients on mTOR inhibitor-containing regimens have a lower incidence of skin cancer and other malignancies than those on calcineurin inhibitors [25-28]. A switch from calcineurin inhibitors to mTOR inhibitors after a first SCC clearly decreases the risk of subsequent SCC in these patients [25].
Clinical and Histopathological Presentation
In immunosuppressed patients, the clinical features of epithelial skin cancer do not greatly differ from those of the general population. However, the differentiation of intraepithelial skin lesions, such as those found in actinic keratosis (AK) and Bowen's disease, from invasive SCC and BCC, respectively, tends to be more difficult.
Due to the immunosuppressive medications taken by OTRs, a reduced amount of inflammation is present in the tumor microenvironments of intraepithelial and invasive skin lesions [11]. Thus, the depth and invasion of skin tumors in OTRs are frequently underestimated by clinical judgment. Hence, the focus on palpation during clinical examination is essential: if a lesion is discretely infiltrated or shows palpable borders or palpable elevation, a biopsy is warranted to rule out invasive skin cancer that may need surgical removal. Tenderness or pain either as a spontaneous observation or as elicited by clinical examination should raise suspicion of the presence of an invasive SCC. A recent study has shown that such tender or painful lesions carry a 75% risk of invasive SCC and should thus be generously biopsied [29]. The reduced immunosurveillance of tumor cells in OTRs has in multiple instances resulted in the rapid development of SCC over a period of weeks, rapid tumor progression and more aggressive tumor behavior in OTRs [30, 31].
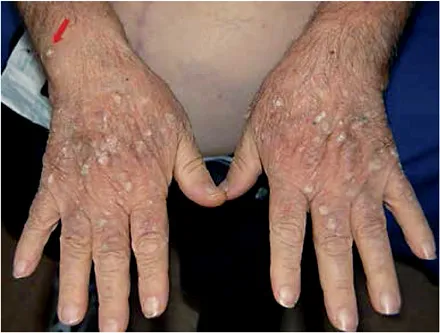
Fig. 1. Multiple hyperkeratotic viral warts, actinic keratosis and one squamous cell carcinoma lesion (arrow) on the hands/forearms of an OTR.
The concept of field cancerization plays an important role in this high-risk population. Generally, sun damage leads to a large number of clinical lesions in OTRs, increasing the need to separate the intraepithelial lesions from the invasive lesions in need of excision [32, 33]. Particularly, in the sun-exposed areas of the skin, such as the balding scalp, face, ears and backs of the hands, multiple AKs, Bowen's disease lesions, and invasive SCC mingle with viral warts and may coexist (fig. 1). The clinical distinction of benign hyperkeratotic lesions from intraepithelial and invasive SCCs is challenging and frequently relies on biopsy for diagnosis.
Few data are available on the histopathology of intraepithelial lesions, such as AKs, in OTRs. Diffuse or focal spindle cell morphology is seen more often in the SCC of OTRs (in up to 20% of these tumors). Bowen's disease may occur multifocally and arise more frequently in sun-protected areas of the body, such as the trunk and anogenital area [11, 31].
Management of Actinic Keratosis in Organ Transplant Recipients by a Dermatologist
Before transplantation, a screening should be performed, and detailed systematic patient education should be provided by the dermatologist. The medical history of risk factors for cutaneous carcino...
Table of contents
- Cover Page
- Front Matter
- Epidemiology of Actinic Keratoses
- Patients’ Perspectives on Actinic Keratosis
- Photodamage: All Signs Lead to Actinic Keratosis and Early Squamous Cell Carcinoma
- Dysregulation of Epidermal Growth Factor Receptor in Actinic Keratosis and Squamous Cell Carcinoma
- The Actinic Keratosis Virome: Can We Prevent Squamous Cell Carcinoma with a Vaccine?
- Do Actinic Keratoses and Superficial Squamous Cell Carcinomas Have a Specific Immunoprofile?
- Mouse Models for Actinic Keratosis and Squamous Cell Carcinoma
- Keratinocyte Cancer and Its Precursors in Organ Transplant Patients
- Clinical Features of Actinic Keratoses and Early Squamous Cell Carcinoma
- The Many Clinico-Pathologic Faces of Actinic Keratosis: An Atlas
- Dermoscopy of Actinic Keratosis, Intraepidermal Carcinoma and Squamous Cell Carcinoma
- The Future of Keratinocyte Skin Cancer Surveillance: Automated Image Analysis to Identify and Monitor Keratinocyte Dysplasia
- Reflectance Confocal Microscopy: Hallmarks of Keratinocyte Cancer and Its Precursors
- Optical Coherence Tomography and Its Role for Delineating the Thickness of Keratinocyte Dysplasia and Neoplasia
- Teledermatology: Its Use in the Detection and Management of Actinic Keratosis
- Conventional Treatment of Actinic Keratosis: An Overview
- Field Cancerization: From Molecular Basis to Selective Field-Directed Management of Actinic Keratosis
- Update on Photodynamic Treatment for Actinic Keratosis
- Laser Treatment and Its Implications for Photodamaged Skin and Actinic Keratosis
- Ingenol Mebutate: From Common Weed to Cancer Cure
- Oral Nicotinamide and Actinic Keratosis: A Supplement Success Story
- Author Index
- Subject Index
Frequently asked questions
Yes, you can cancel anytime from the Subscription tab in your account settings on the Perlego website. Your subscription will stay active until the end of your current billing period. Learn how to cancel your subscription
No, books cannot be downloaded as external files, such as PDFs, for use outside of Perlego. However, you can download books within the Perlego app for offline reading on mobile or tablet. Learn how to download books offline
Perlego offers two plans: Essential and Complete
- Essential is ideal for learners and professionals who enjoy exploring a wide range of subjects. Access the Essential Library with 800,000+ trusted titles and best-sellers across business, personal growth, and the humanities. Includes unlimited reading time and Standard Read Aloud voice.
- Complete: Perfect for advanced learners and researchers needing full, unrestricted access. Unlock 1.4M+ books across hundreds of subjects, including academic and specialized titles. The Complete Plan also includes advanced features like Premium Read Aloud and Research Assistant.
We are an online textbook subscription service, where you can get access to an entire online library for less than the price of a single book per month. With over 1 million books across 990+ topics, we’ve got you covered! Learn about our mission
Look out for the read-aloud symbol on your next book to see if you can listen to it. The read-aloud tool reads text aloud for you, highlighting the text as it is being read. You can pause it, speed it up and slow it down. Learn more about Read Aloud
Yes! You can use the Perlego app on both iOS and Android devices to read anytime, anywhere — even offline. Perfect for commutes or when you’re on the go.
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Please note we cannot support devices running on iOS 13 and Android 7 or earlier. Learn more about using the app
Yes, you can access Actinic Keratosis by H. P. Soyer,T. W. Prow,G. B. E. Jemec,H.P., Soyer,T.W., Prow,G.B.E., Jemec, P. Itin,G. B. E. Jemec,P., Itin,G.B.E., Jemec in PDF and/or ePUB format, as well as other popular books in Medicine & Oncology. We have over one million books available in our catalogue for you to explore.