![]()
Shiohara T (ed): Pathogenesis and Management of Atopic Dermatitis.
Curr Probl Dermatol. Basel, Karger, 2011, vol 41, pp 1-34
______________________
Atopic Dermatitis and the Hygiene Hypothesis Revisited
Carsten Flohr • Lindsey Yeo
Department of Paediatric Dermatology, St. John’s Institute of Dermatology, Guy’s and St. Thomas’ Hospital NHS Foundation Trust and King’s College London, London, UK
______________________
Abstract
Background: We published a systematic review on atopic dermatitis (AD) and the hygiene hypothesis in 2005. Since then, the body of literature has grown significantly. Objectives: We therefore repeated our systematic review to examine the evidence from population-based studies for an association between AD risk and specific infections, childhood immunizations, the use of antibiotics and environmental exposures that lead to a change in microbial burden. Methods: Medline was searched from 1966 until June 2010 to identify relevant studies. Results: We found an additional 49 papers suitable for inclusion. There is evidence to support an inverse relationship between AD and endotoxin, early day care, farm animal and dog exposure in early life. Cat exposure in the presence of skin barrier impairment is positively associated with AD. Helminth infection at least partially protects against AD. This is not the case for viral and bacterial infections, but consumption of unpasteurized farm milk seems protective. Routine childhood vaccinations have no effect on AD risk. The positive association between viral infections and AD found in some studies appears confounded by antibiotic prescription, which has been consistently associated with an increase in AD risk. Conclusions: There is convincing evidence for an inverse relationship between helminth infections and AD but no other pathogens. The protective effect seen with early day care, endotoxin, unpasteurized farm milk and animal exposure is likely to be due to a general increase in exposure to non-pathogenic microbes. This would also explain the risk increase associated with the use of broad-spectrum antibiotics. Future studies should assess skin barrier gene mutation carriage and phenotypic skin barrier impairment, as gene-environment interactions are likely to impact on AD risk.
Copyright © 2011 S. Karger AG, Basel
There has been a dramatic increase in the prevalence of atopic dermatitis (AD) over past decades, currently affecting around 20% of children in developed countries [1]. Although family history plays an important role in AD susceptibility, probably at least partly explained by skin barrier gene mutation carriage, genetics alone cannot explain the increase in AD prevalence [2, 3]. Epidemiological research has therefore focused on identifying possible environmental and lifestyle-related factors that are associated with an increased AD risk. For instance, AD is more common in urban than in rural communities [4]. In addition, migrant studies have demonstrated that immigrants take on the risk of the community to which they move, with AD being more prevalent in western industrialized countries than developing nations [5, 6]. The risk of developing AD is also higher in children growing up in smaller families and families of higher socio-economic status [7-9]. All this strongly suggests an environmental aetiology.
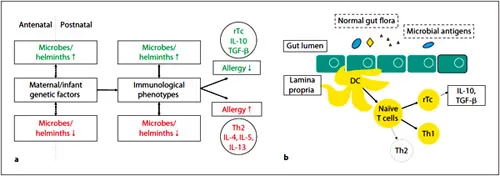
The so-called ‘hygiene hypothesis’ was formulated in the late 1980s, based on the observation that AD and hay fever were noted to be less common among UK children growing up with larger numbers of older siblings [10]. At the time, this was thought to be due to a higher exposure to certain viral and bacterial pathogens in larger families. The hygiene hypothesis has stimulated a large body of both epidemiological and immunological research. For instance, there is evidence from animal models that allergic disease occurs when the developing immune system is deprived of the obligatory stimulation through certain microbial antigens, especially when this happens directly postnatally or even already in utero [11]. Immunologically, this seems partly due to an imbalance between type 1 and type 2 T helper cells and their cytokines. However, the immunological processes ultimately leading to allergic disease are more complex than this. The current hypothesis is that regulatory T cells and anti-inflammatory cytokines such as interleukin 10 and transforming growth factor ß play an important role in the protection against clinical allergy, possibly induced by microbial stimulation of dendritic cells via Toll-like receptors at the level of the gastrointestinal mucosa or other lymphoid tissues (fig. 1a, b) [12-15].
Since our original systematic review on AD and the hygiene hypothesis in 2005, the body of literature has grown significantly, and we therefore decided to revisit this fascinating topic for a second time [16]. We performed a systematic Medline search from inception until June 2010 to address the following questions at the population level: (1) Is there any evidence that the risk of AD is related to environmental exposures that alter microbial burden? (2) Which specific infections have been associated with a reduced AD risk? (3) Is there a link between immunizations, use of antibiotics and AD risk? The online search strategy is available on request from the corresponding author and was supplemented by an extensive hand search of the literature through references identified from retrieved articles. Overall, we identified 49 new studies suitable for inclusion. All studies were analysed qualitatively, and results are presented in summary tables. Where appropriate, we also conducted meta-analyses, namely for pet and antibiotic exposure.
The Link between AD and Environmental Exposures That Can Alter Microbial Burden
Basic hygiene, day care attendance, anthroposophic lifestyle, living on a farm and pets have all been examined as potential risk factors for allergic disease, including AD, since they at least theoretically increase exposure to microbes.
Fig. 1. a Microbial and helminth exposure in utero and postnatally is likely to play an important role in the development of AD. In this model, high exposure burden, probably in interaction with maternal and infant genetic factors, reduces AD risk, whereas AD risk increases if the fetal and/or infantile immune system is deprived of microbial stimulation. The gut mucosa is likely to be a key site for the priming of the immune system (see b). rTc = Regulatory T cells; Th2 = type 2 T helper cells; IL = interleukin;TGF-ß = transforming growth factor ß. b The postulated link between allergic disease and the gut microflora. Chronic stimulation of gut-associated lymphoid tissue through normal gut flora and other non-/pathogenic microbial antigens might ensure the development of a Th1/regulatory T cell-dominated cytokine milieu and therefore prevent clinical expression of allergic disease. Regulatory T cells may have a role in this by the production of anti-inflammatory cytokines, such as IL-10 and TGF-ß. DC = Dendritic cell; Th = T helper cell; rTc = regulatory T cell.
Basic Hygiene
Only one large birth cohort study, the Avon Longitudinal Study of Parents and Children, has so far addressed the question whether cleanliness in terms of general hygiene measures, such as frequency of washing, is associated with an increase in AD risk. Children were seen at 6 and 30-42 months of age, and a moderate increase in AD risk was found with higher levels of personal hygiene, measured as an empirical hygiene score from 1 to 14 (baseline adjusted odds ratio, adj. OR = 1.04, 95% confidence interval, CI = 1.01-1.07; table 1) [17].
Day Care
Three birth cohort studies, one from the USA, one from Denmark and one from Germany, found an inverse relationship between day care attendance and AD, with risk reductions up to 88% (German study adj. OR = 0.12, 95% CI = 0.04-0.31) [18-20]. One ...