![]()
Chapter 1
Clerking Patients
Clerking patients may seem a daunting task initially, but it is an important skill to master. A well performed history and examination allows you to not only reach an appropriate differential diagnosis, and thus request relevant investigations, but also to develop an effective doctor–patient relationship. This chapter will ensure that you structure your history taking, and will point out the important questions to ask. It will help you to focus on understanding symptomatology, common abnormal examination findings and your presentation technique.
1.1 History Taking
It is vital to have a structure, at least in your head, on which to base your history as the patient rarely gives you the information needed in an orderly fashion.
The key cardiac symptoms are:
• Chest pain
• Dyspnoea
• Palpitations
• Oedema
• Syncope
1.1.1 Five simple steps to taking a cardiac history
Step 1: Ask about the presenting complaint:
Also make sure you cover the following, which are the main cardiac symptoms:
• chest pain
• dyspnoea/shortness of breath
• palpitations
• syncope
• oedema.
Bear in mind that none of the above symptoms are cardiac specific; they can be caused by non-cardiac pathology, and therefore thoughtful directed questioning of each symptom can help determine its cause. If a patient presents with any one of these symptoms, do not forget to enquire about the others. Try to keep in mind the causes of each symptom, as this will help direct your questioning.
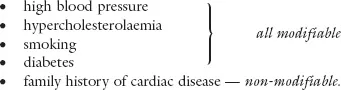
Step 2: Always ask about the five major risk factors, namely:
Step 3: Don't neglect the past medical history, including:
• heart disease and previous cardiac investigations or procedures including angioplasty/stent/bypass grafting
• history of stroke/transient ischaemic attack
• history of peripheral vascular disease
• asthma — as B-blockers and adenosine can cause bronchospasm
• rheumatic fever — predisposition to valve disease
• thyroid disease — can cause palpitations and exacerbate heart failure.
Step 4: A full drug history:
• remember that patients don't often list aspirin or inhalers spontaneously
• any drug allergies? Be specific — patients do not always understand this question. Did the patient have an anaphylactic reaction/ rash/nausea/vomiting, or did they simply not benefit from taking the drug?
Step 5: Patient's social circumstances:
• occupation (for example, taxi drivers and airline pilots have strict occupational health regulations)
• implications post-myocardial infarction
• who lives at home with the patient?
• pre-morbid health — before this admission what was the patient's level of independence and activity? Gives an idea on what to aim for prior to discharge
• alcohol history — predisposition to hypertension, cardiomyopathy and atrial fibrillation.
1.2 Chest Pain
Chest pain is a simple shorthand that we use to describe a wide variety of experiences. You'll be surprised at how often you and the patient may not be referring to the same thing! For example, does the patient mean an ache, heartburn, or heaviness in the chest? Finding out the nature or characteristics of the pain can provide important clues as to whether or not the pain is cardiac in nature.
There are two critical features of cardiac chest pain:
1. Location of the pain may be typically symmetrical across the centre of the chest, potentially including both shoulders and arms, and may radiate up the neck to the jaw. It may be more dominant on the left side.
2. Exertional relationship — coronary pain will always get worse when the patient is physically active. Pain that occurs randomly at rest and during exercise with no exertional link is usually non-cardiac in origin. Pain that has a habitual pattern of only occurring at rest is very unlikely to be cardiac.
Ask about associated shortness of breath and autonomic symptoms such as nausea and sweatiness. Glyceryl trinitrate (GTN) will usually offer some symptom relief, whether the patient is experiencing angina or a myocardial infarction. However, if pain lasts for more than 20 minutes with or without relief by GTN, consideration of a myocardial infarction (MI) is warranted.
1.2.1 The key features of cardiac chest pain
Levine's sign = patient's using a clenched fist to locate the site of the pain.
crushing pain/tightness over central chest
+/− radiation to jaw/down the left arm
+/− autonomic symptoms, for example, nausea, sweatiness
Other cardiac causes of chest pain include:
• Aortic dissection — this is a life-threatening condition where blood is tracking between the layers of the wall of the aorta. Left untreated, there is a high risk of rupture and death. This is characterised by a ‘tearing’ central chest pain radiating to the back between the scapulae. May be accompanied by haemodynamic compromise.
• Pericarditis — this is inflammation of the pericardium which causes chest pain worse on inspiration or lying flat.
• Arrhythmias — these can sometimes cause chest pain if the rate becomes really fast.
The main non-cardiac causes of chest pain that are often mistaken for angina can be divided into respiratory, gastrointestinal and musculoskeletal causes. For example, sharp chest pain is often referred to as pleuritic chest pain and is suggestive of a pleuritic/respiratory cause, such as an infection (for example, pneumonia), inflammation (for example, pleurisy), or infarction (for example, a Pulmonary Embolism [PE]). It is caused by inflamed contact between the lung and pleura.
Some important differentiating questions for pleuritic pain include:
Is it worse on deep inspiration? On coughing? With movement?
Is the pain sharp? Like a sharp knife? Note that some patients will use the word ‘sharp’ to mean ‘severe’ rather than to describe the type of pain.
Consider a gastrointestinal cause such as oesophagitis, oesophageal reflux or spasm if the chest pain is burning and is worse on lying flat or is related to meals. Pain that is relieved on sitting forward may suggest pancreatitis.
Is the pain worse in any one position? Such as lying flat?
Is the pain relieved by sitting forward?
Is the pain worse before/after eating?
Don't forget musculoskeletal/cutaneous chest pain which is confined to the chest wall and may be tender on palpation, for example, Tietz...