![]()
1
Origins of the Epidemic
It began with the death of one little boy. His name was Emile, and he lived in a tiny village in forested Guinea called Meliandou.
His mother, Sia, tried to care for the boys as well as any mother would have, but she, too, soon fell ill, and died, with bleeding symptoms. Sia, who was pregnant, and her mother, were caring for Emile’s sister Philomene, who died shortly thereafter with dark, bloody diarrhea and vomiting. Sia’s mother died next, with symptoms similar to Philomene’s. Two people who attended the grandmother’s funeral returned to their village of Guéckédou, and infected a health care worker and their own family members. By February 2014, the virus had spread to Macenta, Nzérékoré, and Kissidougou.
No one knows how Emile contracted EVD in December. Perhaps he was fed some bushmeat, such as meat from a fruit bat. Some thought perhaps a vector of some kind, a tick, or a flea, injected the virus into his body. A report in December 2014 indicated that he had played under a tree that harbored an insectivorous bat species. Regardless of how he contracted it, no one in Emile’s village of Meliandou could have suspected EVD. Their community resides deep in the forested area of Guinea, where many other culprits, such as cholera, typhoid, and Lassa fever, could have explained his symptoms. The infant death rate in Guinea is 10 times as high compared to that in the United States, and is especially high in the isolated areas, where there are few hospitals and doctors. The village is located near the nexus of a border with remote areas of two other countries: Sierra Leone and Liberia. Cross-border trade among locals in these countries is routine; the people in these remote areas in the three countries feel and share kinship regardless of national border, carrying the virus with them. For months, the virus spread through families and villages and borders traveling quickly on improved roads. As people fell ill, their family members cared for them. Sick children were carried by their parents; older children were moved to hospitals in wheelbarrows. The virus’ aim was deadly, killing over 90% of its victims.
Four months later, in March, 2014, nearly 4,000 miles away, central processing units spinning electrons in computers at Children’s Hospital in Boston picked up blips suggesting a “mystery hemorrhagic fever” in forested areas of southeastern Guinea. Nine days would pass before the WHO doctors could recognize the uptick in deaths, and finally sound the alarm: Ebola.
Four months had passed between Emile’s death and the WHO announcement of an outbreak of Ebola. Four months is an unusually long incubation period for Ebola to be passed among locals without detection. In the past, outbreaks had typically been localized, with a high fatality rate, and they were recognizable in part due to hemorrhaging and a high mortality rate. The symptoms had been characteristic and increasing in severity: fever, aches, pains, vomiting, diarrhea, and then exhaustion, followed by body rash, and coma via loss of blood pressure shock. During the Sudan Ebola quasispecies outbreak in the Democratic Republic of the Congo, 76 people got sick, of whom 59 died. These outbreaks had, in the past, been recognizable in part due to hemorrhaging. High prevalence of typical tell-tale bleeding from eyes, ears, nose and mouth gave the disease its traditional name: “Ebola hemorrhagic fever” (EHF).” We know now that this occurred as a result of more and more cells producing more and more virus particles, especially white blood cells (Wauquier et al., 2010), causing the immune system unleashes a last-ditch “cytokine storm,” which itself does massive tissue damage. As the disease spread in early 2014, the doctors treating patients starting dying, and hospitals in the provincial towns of Guéckédou and Macenta (Fig. 1.1) may have been more likely to correctly diagnose their patients, and themselves; however, somehow they, too missed the signs of Ebola. Perhaps they, too, considered cholera, malaria, or other types of fevers from the region with similar symptoms. It now seems that there was less bleeding.
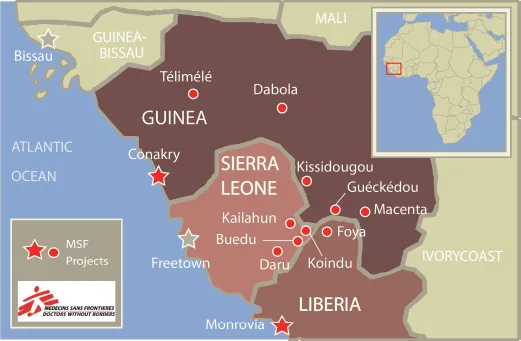
Fig. 1.1 Map of Western African countries at the center of the epidemic. Capital cities and Doctors Without Borders Project (MSF) sites are shown. “Ground Zero” village Meliandou, where Emile and his family lived at the onset of the 2013/2014 Ebola crisis, lies east of Guéckédou. Image credit: © 2014, MSF. Used with permission. http://www.msf.ca/en/article/ebola-west-africa-epidemic-out-control.
Early in the outbreak, certainly no one in the region expected Ebola. No county in Western Africa had seen an outbreak of EVD. According to Dr. Margaret Chan, Director-General of the World Health Organization (WHO), the ecological conditions, the wildlife species (fauna), and hunting practices, that are ripe for a zoonotic transfer of Ebolavirus to humans exist in 22 African countries. So far, outbreaks had occurred in only five African countries: Democratic Republic of the Congo (Zaire), Uganda, Gabon, Sudan, and Ivory Coast.
Even if they had somehow known that this region was afflicted with EVD, their description of the emergence of EVD in West Africa would have included a key discrepancy in their observation from past outbreaks: While most patients suffered from fever, vomiting and severe diarrhea, fewer (~40%) suffered from visible hemorrhaging. Compared to the first EHF outbreak of the Sudan virus, in 1976:
Haemorrhagic manifestations were common (71%), being present in half of the recovered cases and in almost all the fatal cases.
(WHO Bull, World Health Organization 1978; 56(2): 247–70)
This statistic is important, but is rarely referenced. The number of health care workers that were becoming infected was very high; by August, over 216 health care workers had died. Around 5% of all cases in this outbreak have been health care workers. This is in the context in some countries in which there are very few doctors. In Guinea, the country in which the epidemic began as an outbreak, there are only 0.1 doctors per 1,000 people; in Sierra Leone, 0.022; in Liberia, about 0.014 (WHO). In the US, there are about 2.5 doctors/1000 people. In fact the WHO reports that 45.8% of WHO member states report to have less than one physician per 1,000 people. The death rates among the infected were initially very high (>90%); these have tapered now to just >50%. The losses of health care workers represent the virus fighting back directly against the health care system, which in some of the poorest areas of these countries, is virtually non-existent. The virus attacks everything we throw at it: In December 2014 we learned that some UN peacekeepers had contracted EVD. Transmission is thus far understood to require direct contact of Ebolavirus with a mucous membrane, either in the eye, mouth, or nose. However, to understand transmission risks of an infectious agent, one must have an understanding of the biology of the virus.
Perhaps the single largest factor contributing the initial exponential spread of the virus remains: The international global response was deplorable. The urgency communicated by WHO officials and some at the UN has been described as frantic; they were literally screaming that no one understood the seriousness of this outbreak. Dr. Tom Frieden, Director of the CDC, was among the earliest voices with a clarion call to pay attention to this particular outbreak. The lag in the international response was not likely due to complacency; between outbreaks, the WHO and the CDC witness many false positive alarms for infectious disease outbreaks and, like cancer treatment, “watchful waiting” often is the standard protocol. It seems no protocol is in place to attempt to rapidly ground-truth each and every possible report. The WHO held an international meeting and concluded that a vaccine was desperately needed, as a first priority. The Obama administration’s response to the pleas for help included plans for Domestic Preparedness and pledges of aid to Ebola-affected countries. This has included use of US troops to build hospitals.
The international response has increased in response to the size and duration of the epidemic. In Jan 2015, China added 232 army medical workers to the 43 army doctors and 35 specialists from their CDC.
The most vocal critics of the US response to the crisis first came in the form of interrogation by Congressional Representatives in House Oversight hearings at the US Capitol. Over the course of a few days, the principle leaders of institutions in the US at the fore-front of the outbreak — the CDC, the NIH, the NIAID, and Major General James Lariviere, deputy director of political-military affairs in Africa for the Defense Department, were questioned about everything from the nature of the threat to the misleading information provided by the CDC on their website. There was a mid-term election coming, and the air was thick with finger pointing and politicization of a grave topic. Senators were visibly agitated, and panelists were, at times, literally shaking.
DHS Inspector General John Roth testified that while the agencies in question had purchased antivirals and PPE, there was no fully developed understanding of what an epidemic of this sort would require, and no plans for who would receive what supplies. Others testified that airport screening was not working. At the time, new cases of EVD were being announced even as the hearings proceeded.
Senator Chuck Grassley (IA) commented that he was “scared to death of Ebola,” and later introduced a bill banning visas for people living in Ebola-affected countries. Congressional Representative Fred Upton (MI) asked CDC director Thomas Frieden why there was no fail-safe ban on people traveling from affected countries. Dr. Frieden’s reply was that a ban would prevent them from tracing possible cases, to which Representative Fred Upton quipped: “ We should not let them in … period.” Speaking with reporters after the hearings, Representative Cory Gardner (CO) took Dr. Frieden to task for his reasoning: “That’s like saying all children with chicken pox should stay in school so we know where they are.” Representative Tim Murphy (PA) told news host Chris Wallace that he did not thinks “false assurances” were working. An epidemiologist, Dr. Vera F. Dolan, provided an affidavit citing the studies of experimental aerosol transmission in monkeys and suspected aerosol transmission in pigs as evidence for her support of enforced 21-day quarantine and travel restrictions. She wrote:
In my opinion, any individual who has visited the Ebola-affected African countries of Guinea, Sierra Leone, and Liberia should be quarantined for 21 days. Such individuals should be put on a “no-f ly” list, to be kept in force until the officially declared end of the current Ebola epidemic.
— Mendocino County, CA, Court Affidavit, Oct 10, 2014
The NIH and the CDC have sought to reassure the American public that it is extremely unlikely that an epidemic of the type seen in Western African could happen in the US. They have confidence in our ability to identify any cases, and shut down any transmission chains. However, the experiences in the late summer and autumn of 2014 did anything but reassure many. The US did not seem ready.
In fact, we were not. Another sign of the CDC’s lack of readiness for an epidemic of this scale is that the software for Ebola data collection was designed so only a single person could enter data at a time. The CDC was not quite ready to track people large numbers of people. The system was updated for multiple people to enter data; however, some wonder why the CDC is writing software in the first place. To guarantee state of the art data collection, companies like Apple and Microsoft could design apps and provide hardware that uses state of the art wireless technologies. This type of oversight in preparedness had led some to describe the US response as “clumsy” (Johnson, 2014).
Back in Western Africa, any and every bit of help in any form was then, and still is needed. In Sierra Leone, especially, it seems as of this writing, if every country and company gave all, it still might not be enough.
The Wee Beastie
Ebola is a terrifying monster. Its genome is devastatingly brilliant, seemingly designed like a monkey puzzle tree. Under the right terrifying conditions, it has the capacity to kill millions in a few months’ time. While policy makers in the US ponder how wrong it would be to close our borders to reduce the risk of it spreading here, this virus has already closed borders in numerous African countries; it is waging war on their economies and the psyche of their peoples; it has brought the world media’s attention and focus away from the threat of a third world war (the Ukraine crisis), and it shows no sign of stopping in spite of a massive, concerted international effort.
The human genome has some 47,000 known and suspected (predicted) genes.
This Thing has a mere seven protein-coding genes.
Genes translated into proteins in human cells are encoded by a simple alphabet of four letters: A, T, C, and G. Any combination of three of these letters encodes an encrypted word (codon), which, is then translated by special proteins in the cell (ribosomes) into a word (amino acid). ...