![]()
Chapter 1
Automating the Perioperative Process
1.1Background
The perioperative setting is the most resource intensive section of the hospital, accounting for about half of the hospitals budget. Any improvements in quality care and operational efficiency in the perioperative process would enhance the hospitals ability to meet budget targets. A hospital’s perioperative department’s performance also impacts patient safety. Approached systemically, patient throughput, surgical instrument identification and count, sterilization, and room turns can be dramatically improved.
On May 3, 2011, the standing Committee on Veterans Affairs in the United States House of Representatives held a hearing titled: “Sacred Obligation, Restoring Veteran Trust and Patient Safety.” This hearing was initiated due to incidents of serious patient safety violations in VA medical facilities across the United States in Dayton, St. Louis, and Miami resulting in thousands of veterans across the country receiving notification of their potential risk for infectious diseases like the human immunodeficiency virus (HIV) and hepatitis.
The sterilization issues were mainly attributed to ineffective sterilization of reusable medical equipment (e.g., ear, nose, and throat endoscopes). The causes for these lapses in sterilization include:
•Inadequately trained staff; failure to develop device-specific training requirements.
•Trained staff with potential lapses in performance.
•Number of devices and brand types currently used across the different facilities.
•Lack of quality control
•Lack of effective oversight
These lapses pose potential risks to the safety of veterans. Automating the sterilization process will reduce the extent of human involvement in the process, reducing potential safety risks.
1.2Current Perioperative Process
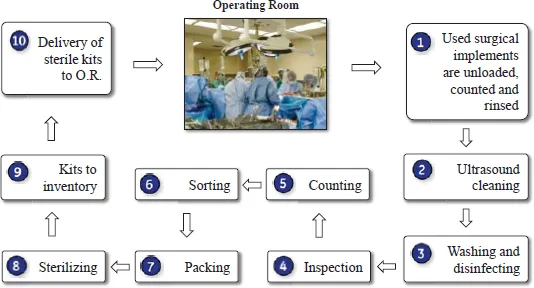
Fig. 1.1 The current perioperative process in VA medical facilities.
Fig. 1.1 shows the current steps of perioperative processing in VA medical facilities. The logistics of sterilizing, sorting, building, transporting, and counting sterile instruments is labor and capital intensive. Processing hundreds of types of instruments with very similar characteristics requires an extensive learning curve for hospital employees and perfect human diligence. Instruments and kits arrive in the dirty side of the sterilization room, where they are manually unloaded, counted, rinsed (Step 1). Then, they are cleaned in an ultrasonic cleaning system (Step 2). The washer/disinfector physically separates the dirty side of the sterilization room from the clean side (Step 3). The instruments are then removed from the washer/disinfector from the clean side, where they are inspected, counted, sorted, packed, and sterilized (Steps 48). The sterile kits are stored in inventory until needed (Step 9). The sterile kits are finally taken from inventory and delivered to the Operating Room (OR) (Step 10). The inventory and ORs are in a remote location from the sterilization room and may even be on a different floor of the hospital. The sterilization process directly affects the hospitals main profit center-the OR. Common mistakes made in the sterilization and delivery process such as incorrect kit constructs, counting errors, broken instruments, and un-sterile equipment affect patient safety, scheduling, throughput, and capacity in the OR.
1.3Our Goal
To address this problem, we proposed an integrated system solution. Robotics, conveyors, auto-ID, and computer vision technologies are integrated to perform the sterilization steps. With the automated sterilization and delivery process, our main goal is to achieve increased safety, improved perioperative throughput, and enhanced care quality.
1.3.1Increased Safety
The primary benefit from this automated solution is the development of a less manual process that reduces errors in the process and sub-standard sterilized instruments. By reducing human handling, we will increase the safety of the patients.
1.3.2Improved Throughput
This automated solution will also increase the efficiency in OR scheduling due to increased kit accuracy and reduction in instrument counting time. In addition, by integrating automatic instrument tracking, handling, and sterilization together in a systemic way, we will enable more instrument throughput while improving on overall performance such as correct delivery.
1.3.3Enhanced Care Quality
By implementing our automated solution, we can increase hospital quality and budget performance through reduction in surgical infections. We can also increase hospital capacity by reducing infection rates that require longer in-patient stays and by reducing operation set-up and room turn-around time. In the long term, improved staff to patient ratio will also have a significant impact on the quality of the care.
1.4Our Approach
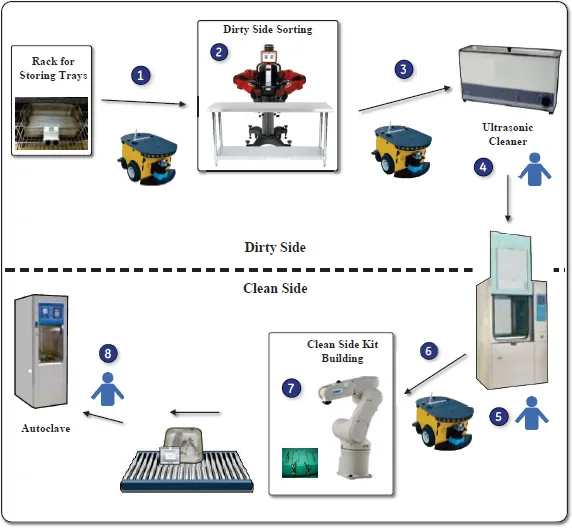
Fig. 1.2 shows a diagram of our proposed automated, integrated sterilization and instrument delivery process. We decided to focus our efforts on the sterilization room because robots are already widely used in hospitals to transport clinical supplies. TUG, a delivering robot manufactured by Aethon [Aethon (2018)], was already used in 27 VA facilities at the time of project initiation. Thus, our process does not include either delivering dirty instruments from ORs to sterilization process nor delivering sterilized surgical kits to storage room.
Before our automated process starts, wire trays containing dirty surgical instruments are returned from ORs and placed on a cart. Then, these surgical instruments are sorted, counted, inspected, and washed on the dirty side of the sterilization room. Then, instruments are disinfected before entering into the clean side of the sterilization room. At the clean side, our robot places the surgical instruments into surgical kits based on the requests logged in the information management system. Finally the surgical kits are wrapped and placed into autoclave for sterilization. The remaining of this section discusses each step in more details.
Fig. 1.2 Automated, integrated sterilization and delivery process. Among all the steps, steps 1, 2, 3,6, and 7 are performed by our robots. Steps 4, 5, 8 are performed by sterile processing nurses.
1.4.1Move Dirty Instrument to Sorting Table - Step 1
At the beginning of our automated process, the dirty surgical instruments are returned back from OR and randomly placed in instrument trays. The trays are then placed on a cart. We developed a mobile robotic system called TrayBot using an Adept Mobilrobots PowerBot [Adept Mobilerobots (2016)] equipped with a 6-DOF Schunk® PowerCube arm. We enhanced each tray with a customer designed handle. On top of the handle, there is a 2D fiducial marker, which serves as the ID of the tray. The down-looking camera on the PowerCube arm can detect the location and orientation of the fiducial marker. The tray can then be picked up by the arm using our customized end effector. TrayBot then navigates itself around the dirty side of the sterilization processing center and places the tray on the sorting table. Fig. 1.3 shows a picture of the Traybot, how Traybot approaches and picks up the dirty instrument tray, a picture of the tray with a handle, and how Traybot grasps the tray by the attachment.
Fig. 1.3 a) Picture of our TrayBot. b) TrayBot reaches for a tray on the cart. c) Picture of a tray and its attachment with a 2D fiducial marker printed on it. d) TrayBot grasps the tray by the attachment using our self-aligning gripper.
Fig. 1.4 a) A picture of Baxter sorting instruments from an unordered pile. b) The instruments are sorted into three trays based on their types by the Baxter.
1.4.2Sort the Instruments - Step 2
After the dirty instrument trays are placed on the sorting table, they are sorted into separate trays based on their types (e.g., tweezers, scissors, etc.). This is to facilitate the ultrasonic washing step because different types of instruments require different scrubbing and washing procedures. Another purpose of this step is to identify each instrument and perform instrument tracking function. We developed a low cost sorting solution using a Baxter robot from RethinkRobotics® [Rethink Robotics (2018)]. The Baxter is equipped with a high definition camera for surgical instrument identification and pose estimation. A customer designed electromagnetic end effector is used pick and place the instruments.
Fig. 1.4 shows the a picture of Baxter and picture of the three sorted trays after sorting at the dirty side.
1.4.3Move Sorted Instruments to Cleaner - Step 3
After Baxter sorts the dirty instruments into multiple trays based on instrument type, Traybot picks them up from the so...