Creating Effective Mental and Primary Health Care Teams provides the practical information, skills, and clinical approaches needed to implement an integrated collaborative care program and support the members of the care team as they learn this new, evidence-based, legislatively mandated care delivery system. Unique in presenting information specifically designed to be used in an integrated, collaborative care workflow, this book provides specific guidance for each member of the team. Care managers, consulting psychiatrists, primary care providers, and administrators alike can finally get on the same page in regard to patient care by referring to the same resource and employing a common framework. Written by recognized experts with broad research, clinical, implementation, and training experience, this book provides a complete solution to the problem of fragmented care.
Escalating costs and federal legislation expanding access to healthcare are forcing the industry to transition to a new model of health care delivery. This book provides guidance on navigating the changes as a team to provide the best possible patient care.
- Integrate physical and behavioral care
- Use evidence-based treatments for both
- Exploit leading-edge technology for patient management
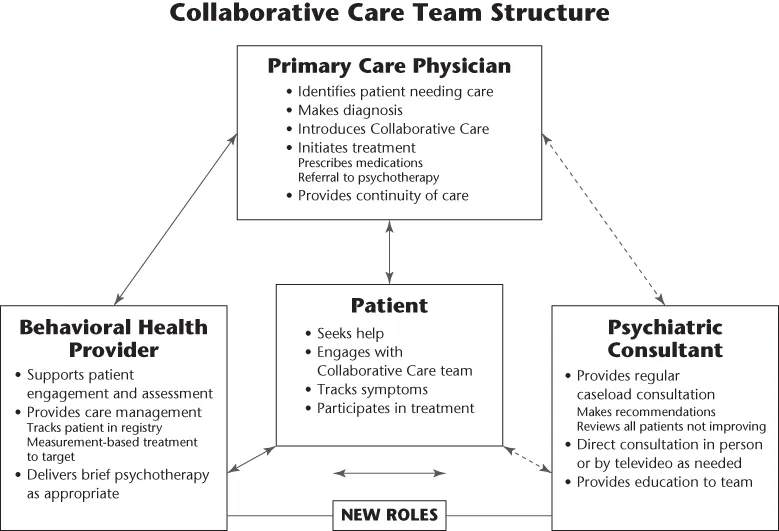
- Support each member of the collaborative care team
Strong evidence has demonstrated the efficacy of a collaborative care approach for delivering mental health care to patients in a primary care setting. The field is rapidly growing, but few resources are available and working models are limited. This book provides a roadmap for transitioning from traditional methods of health care to the new integrated model. Providers ready to move to the next level of care will find Creating Effective Mental and Primary Health Care Teams an invaluable resource.