![]()
Chapter 1
Cardiac Arrest and the Chain of Survival
Jasmeet Soar1, Gavin D. Perkins2, and Jerry Nolan3
1Southmead Hospital, North Bristol NHS Trust, Bristol, UK
2Warwick Medical School, University of Warwick, Coventry, UK
3Royal United Hospital, Bath, UK
OVERVIEW
- Cardiovascular disease is the commonest cause of cardiac arrest
- Early recognition of warning signs and a call for help can prevent cardiac arrest
- If cardiac arrest occurs, immediate cardiopulmonary resuscitation (CPR) improves chances of survival
- Shockable cardiac arrest rhythms (ventricular fibrillation/pulseless ventricular tachycardia, VF/VT) are treated with attempted defibrillation
- Non-shockable rhythms (asystole and pulseless electrical activity (PEA)) are treated by identifying and treating the underlying cause.
- Post-cardiac arrest care in successfully resuscitated patients determines the final outcome
Epidemiology of cardiac arrest
In 2006, coronary heart disease accounted for 1 of every 6 deaths (a total of 425,425) in the United States and one-third of these deaths occurred within 1 h of symptom onset. In Europe, the annual incidence of emergency medical system (EMS)-treated, out-of-hospital cardiopulmonary arrest (OHCAs) for all rhythms is 40 per 100,000 population, with ventricular fibrillation (VF) arrest accounting for about one-third of these. However, data from recent studies indicate that the incidence of VF is declining: it was reported most recently as 23.7% among EMS-treated arrests of cardiac cause. Survival to hospital discharge is 8–10% for all-rhythm and around 21–27% for VF cardiac arrest; however, there is considerable regional variation in outcome.
The incidence of in-hospital cardiac arrest (IHCA) is difficult to assess because it is influenced heavily by factors such as the criteria for hospital admission and implementation of a Do Not Attempt Resuscitation (DNAR) policy. There are an estimated 200,000 treated IHCAs each year in the United States—approximately one per 1000 bed days. Of these patients undergoing CPR, 17.6% survive to hospital discharge and 13.6% have a favourable neurological outcome (Cerebral Performance Category (CPC) 1 or 2). Many patients sustaining an IHCA have significant comorbidity, which influences the initial rhythm and, in these cases, strategies to prevent cardiac arrest are particularly important.
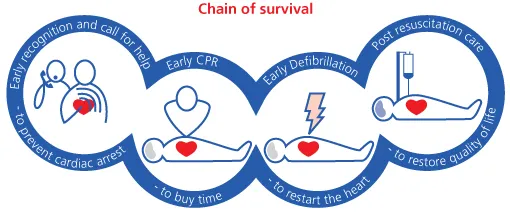
The chain of survival
The key steps for improving survival are shown in the chain of survival (Figure 1.1).
Early recognition and call for help
Out-of-hospital, early recognition of the importance of chest pain will enable the victim or a bystander to call the EMS and the victim to receive treatment that may prevent cardiac arrest. In-hospital, early recognition of the deteriorating patient who is at risk of cardiac arrest and a call for the resuscitation team or medical emergency team (MET) will enable treatment to prevent cardiac arrest. If cardiac arrest occurs, early recognition and a call for help are essential. Agonal breathing (gasping) often occurs immediately after cardiac arrest and is often mistaken for a sign of life—this can cause delays in starting CPR.
Early CPR
If cardiac arrest occurs, the victim will be unconscious, unresponsive and not breathing or not breathing normally (agonal breathing). Cardiopulmonary resuscitation (CPR) with chest compressions and ventilation of the victim's lungs will slow the deterioration of the brain and heart. Bystander CPR doubles the chances of long-term survival. Interruptions to chest compressions must be minimised and should occur only briefly during defibrillation attempts and rhythm checks.
Early defibrillation
Ventricular fibrillation (VF) is the commonest initial rhythm after a primary cardiac arrest although this often deteriorates to a non-shockable rhythm by the time it is first monitored. Early defibrillation can be effective at restoring a circulation. Public Access Defibrillation (PAD) programs using automated external defibrillators (AEDs) enable a wide range of rescuers to treat OHCA caused by VF. Most IHCAs tend to have an initial rhythm of pulseless electrical activity (PEA) or asystole but most survivors are among those with VF arrest. Hospital staff should therefore be trained and authorised to use a defibrillator (AED or manual) to enable the first responder to a cardiac arrest to attempt defibrillation when indicated, without delay.
Post resuscitation care
Return of a spontaneous circulation (ROSC) is an important phase in the continuum of resuscitation; however, the ultimate goal is a patient with normal cerebral function, a stable cardiac rhythm and normal haemodynamic function, so that they can leave hospital in good health and at minimum risk of a further cardiac arrest. The quality of the treatment given in the post-cardiac arrest phase will influence outcome—there is considerable inter-hospital variation in outcome among patients admitted to an intensive care unit after cardiac arrest (Box 1.1).
Box 1.1 Cardiac arrest statistics for the UK
- Over 50,000 out-of-hospital cardiac arrests attended by the ambulance service
- About one-third of cardiac arrest victims have bystander CPR before an ambulance crew arrives
- About 30,000 in-hospital cardiac arrests each year
- Survival to discharge for out-of-hospital cardiac arrests is <10%
- Survival to discharge for in-hospital cardiac arrests is 10–20%
Resuscitation guidelines
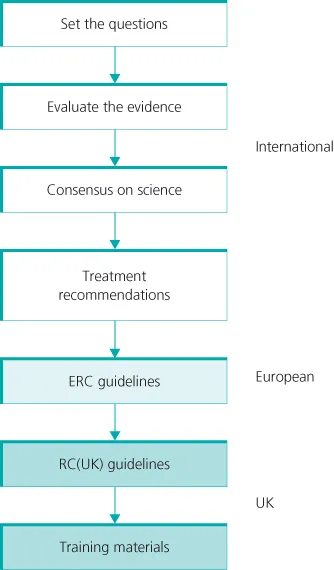
The Resuscitation Council (UK) (www.resus.org.uk) provides healthcare professionals and laypeople with evidence-based guidelines for all patient groups (adults, children, newborn) and all settings. The scientific evidence supporting these guidelines is reviewed every 5 years (most recently in 2010). The UK Guidelines are based on the European Resuscitation Council (www.erc.edu) Guidelines. The European Guidelines are in turn derived from the International Liaison Committee on Resuscitation (ILCOR) Consensus on Science and Treatment Recommendations (CoSTR). ILCOR (www.ilcor.org) therefore establishes the scientific evidence for the guidance and creates treatment recommendations (Figure 1.2).
Further Reading
Meaney PA, Nadkarni VM, Kern KB, et al. Rhythms and outcomes of adult in-hospital cardiac arrest. Crit Care Med 2010;38:101–8.
Merchant RM, Yang L, Becker LB, et al. Incidence of treated cardiac arrest in hospitalized patients in the United States. Crit Care Med 2011;39:2401–6.
Nichol G, Thomas E, Callaway CW, et al. Regional variation in out-of-hospital cardiac arrest incidence and outcome. JAMA 2008;300:1423–31.
Nolan JP, Soar J, Zideman DA, et al. on behalf of the ERC Guidelines Writing Group. European Resuscitation Council Guidelines for Resuscitation 2010: Section 1. Executive summary. Resuscitation 2010;81:219–76.
Nolan JP, Hazinski MF, Billi JE, et al. Part 1: Executive summary: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Resuscitation 2010 Oct;81(Suppl 1):e1–25.
Nolan J, Soar J, Eikeland H. The chain of survival. Resuscitation 2006;71:270–1.
Resuscitation Council (UK). Resuscitation Guidelines 2010. Available at http://www.resus.org.uk/pages/guide.htm.
Sasson C, Rogers MA, Dahl J, Kellermann AL. Predictors of survival from out-of-hospital cardiac arrest: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcomes 2010;3:63–81.
![]()
Chapter 2
Sudden Cardiac Death
David Pitcher
University Hospital Birmingham, UK
OVERVIEW
- SCD can occur at any age, but its frequency increases with increasing age and its causes vary with age
- Ischaemic heart disease is the commonest cause of SCD in people older than 35 years
- Inherited conditions are more common in people below the age of 35
- Warning signs are often absent, but can include chest pain, shortness of breath and syncope
- Identification and treatment of the underlying condition under specialist guidance can prevent SCD
Introduction
Sudden cardiac death (SCD) is defined as ‘Natural death due to cardiac causes, heralded by abrupt loss of consciousness within 1 hour of the onset of acute symptoms; pre-e...